Book traversal links for 2.7.1 Summary of evidence and rationale
Several clinical characteristics, conditions and comorbidities can indicate an increased risk for developing TB disease or suffering worse outcomes from the disease, or both. Individuals identified as having untreated fibrotic lesions on CXR and who are not diagnosed with TB disease are at increased risk of developing TB disease (34–37). These individuals are often identified through TB screening or clinical evaluation or during a clinical evaluation done for other reasons. Individuals with other risk factors for TB or risk factors for poor outcomes from TB often can be identified most easily in health care settings (38–66). Table 2 summarizes the evidence about the primary risk factors for TB and for poor health outcomes related to TB. Groups with other risk factors – such as people with malignancies and other disorders that compromise their immune system and people receiving immunomodulatory therapies – may also be prioritized, depending on the local epidemiology and capacity of the health system.
This recommendation has not been changed from the 2013 guidelines because since the last GDG meeting, no new, robust evidence was found about the impact of systematic screening for TB disease compared with passive case-finding for screening of individuals with risk factors.
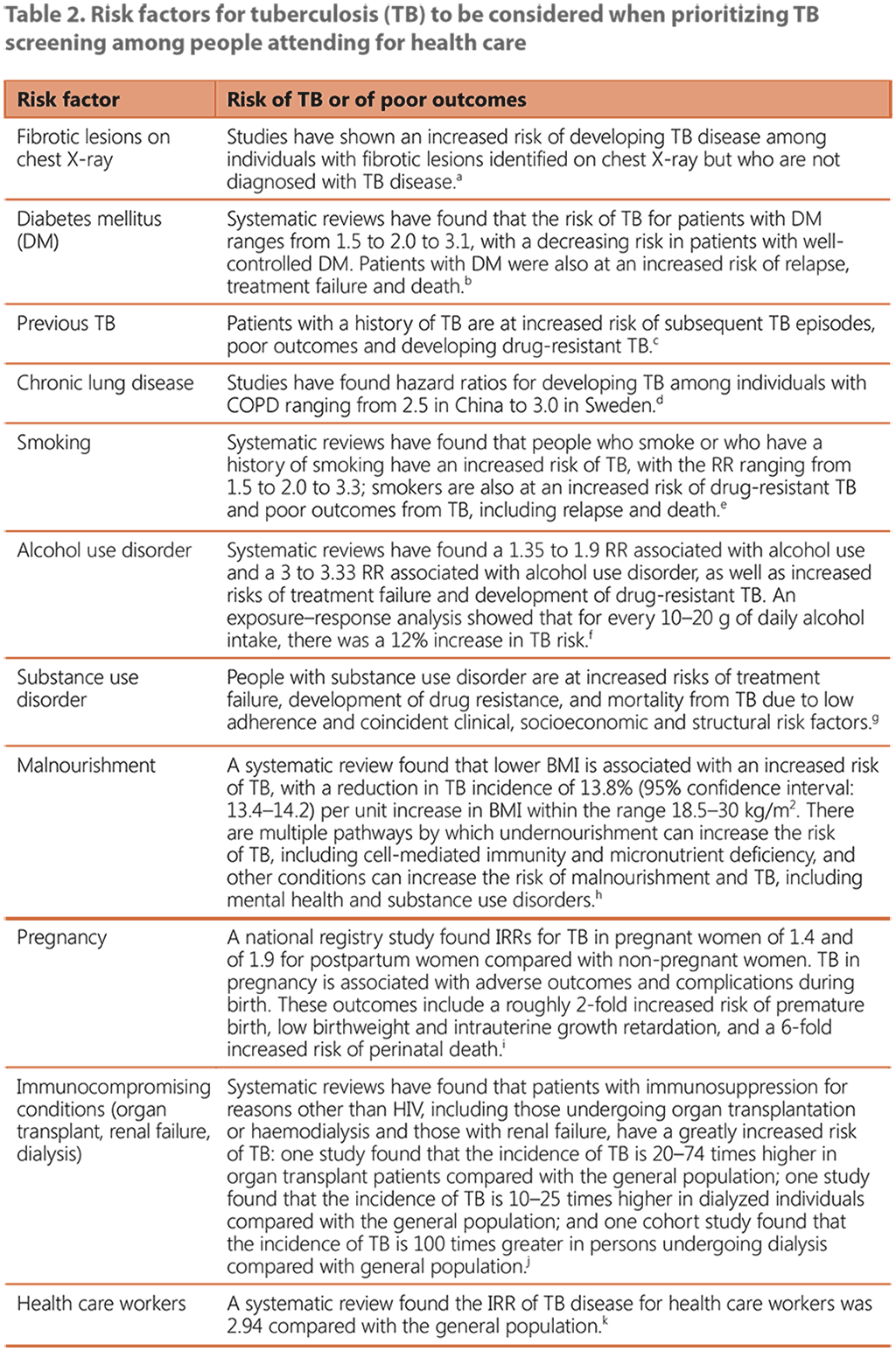
BMI: body mass index; COPD: chronic obstructive pulmonary disease; DM: diabetes mellitus; IRR: incidence rate ratio; RR: relative risk.
ᵃ Ferebee SH. Controlled chemoprophylaxis trials in tuberculosis. A general review. Bibl Tuberc. 1970;26:28–106. Meijer J, Barnett GD, Kubík A, Stýblo K. Identification des sources d’infection [Identification of sources of infection]. Bull Int Union Tuberc. 1971;45:5–54. Okada K, Onozaki I, Yamada N, Yoshiyama T, Miura T, Saint S, et al. Epidemiological impact of mass tuberculosis screening: a 2-year follow-up after a national prevalence survey. Int J Tuberc Lung Dis. 2012;16:1619–24. doi:10.5588/ijtld.12.0201. Gao L, Li X, Liu J, Wang X, Lu W, Bai L, et al. Incidence of active tuberculosis in individuals with latent tuberculosis infection in rural China: follow-up results of a population-based, multicentre, prospective cohort study. Lancet Infect Dis. 2017;17:1053–61. doi:10.1016/s1473–3099(17)30402–4.
ᵇ Hayashi S, Chandramohan D. Risk of active tuberculosis among people with diabetes mellitus: systematic review and meta-analysis. Trop Med Int Health. 2018;23:1058–70. doi:10.1111/tmi.13133. Al-Rifai RH, Pearson F, Critchley JA, Abu-Raddad LJ. Association between diabetes mellitus and active tuberculosis: a systematic review and meta-analysis. PLOS ONE. 2017;12:e0187967. doi:10.1371/journal.pone.0187967. Harries AD, Kumar AM, Satyanarayana S, Lin Y, Zachariah R, Lönnroth K, et al. Addressing diabetes mellitus as part of the strategy for ending TB. Trans R Soc Trop Med Hyg. 2016;110:173–9. doi:10.1093/trstmh/trv111. Baker MA, Harries AD, Jeon CY, Hart JE, Kapur A, Lönnroth K, et al. The impact of diabetes on tuberculosis treatment outcomes: a systematic review. BMC Med. 2011;9:81. doi:10.1186/1741–7015–9-81.
ᶜ Zignol M, Wright A, Jaramillo E, Nunn P, Raviglione MC. Patients with previously treated tuberculosis no longer neglected. Clin Infect Dis. 2007;44:61–4. doi:10.1086/509328. Lambert ML, Hasker E, Van Deun A, Roberfroid D, Boelaert M, Van der Stuyft P. Recurrence in tuberculosis: relapse or reinfection? Lancet Infect Dis. 2003;3:282–7. doi:10.1016/s1473–3099(03)00607–8. Verver S, Warren RM, Beyers N, Richardson M, van der Spuy GD, Borgdorff MW, et al. Rate of reinfection tuberculosis after successful treatment is higher than rate of new tuberculosis. Am J Respir Crit Care Med. 2005;171:1430–5. doi:10.1164/rccm.200409–1200OC. Osman M, Welte A, Dunbar R, Brown R, Hoddinott G, Hesseling AC, et al. Morbidity and mortality up to 5 years post tuberculosis treatment in South Africa: a pilot study. Int J Infect Dis. 2019;85:57–63. doi:10.1016/j.ijid.2019.05.024.
ᵈ Inghammar M, Ekbom A, Engström G, Ljungberg B, Romanus V, Löfdahl CG, et al. COPD and the risk of tuberculosis–a population-based cohort study. PLOS ONE. 2010;5:e10138. doi:10.1371/journal.pone.0010138. Lee CH, Lee MC, Shu CC, Lim CS, Wang JY, Lee LN et al. Risk factors for pulmonary tuberculosis in patients with chronic obstructive airway disease in Taiwan: a nationwide cohort study. BMC Infect Dis. 2013;13:194. doi: 10.1186/1471-2334-13-194.
ᵉ Jayes L, Haslam PL, Gratziou CG, Powell P, Britton J, Vardavas C, et al. SmokeHaz: systematic reviews and meta-analyses of the effects of smoking on respiratory health. Chest. 2016;150:164–79. doi:10.1016/j.chest.2016.03.060. Lin HH, Ezzati M, Murray M. Tobacco smoke, indoor air pollution and tuberculosis: a systematic review and meta-analysis. PLOS Med. 2007;4:e20. doi:10.1371/journal.pmed.0040020. Wang MG, Huang WW, Wang Y, Zhang YX, Zhang MM, Wu SQ, et al. Association between tobacco smoking and drug-resistant tuberculosis. Infect Drug Resist. 2018;11:873–87. doi:10.2147/idr.s164596. Alavi-Naini R, Sharifi-Mood B, Metanat M. Association between tuberculosis and smoking. Int J High Risk Behav Addict. 2012;1:71–4. doi:10.5812/ijhrba.5215.
ᶠ Imtiaz S, Shield KD, Roerecke M, Samokhvalov AV, Lönnroth K, Rehm J. Alcohol consumption as a risk factor for tuberculosis: metaanalyses and burden of disease. Eur Respir J. 2017;50:1700216. doi:10.1183/13993003.00216–2017. Simou E, Britton J, Leonardi-Bee J. Alcohol consumption and risk of tuberculosis: a systematic review and meta-analysis. Int J Tuberc Lung Dis. 2018;22:1277–85. doi:10.5588/ ijtld.18.0092. Rehm J, Samokhvalov AV, Neuman MG, Room R, Parry C, Lönnroth K, et al. The association between alcohol use, alcohol use disorders and tuberculosis (TB). A systematic review. BMC Public Health. 2009;9:450. doi:10.1186/1471–2458–9-450.
ᵍ Deiss RG, Rodwell TC, Garfein RS. Tuberculosis and illicit drug use: review and update. Clin Infect Dis. 2009;48:72–82. doi:10.1086/594126. Getahun H, Gunneberg C, Sculier D, Verster A, Raviglione M. Tuberculosis and HIV in people who inject drugs: evidence for action for tuberculosis, HIV, prison and harm reduction services. Curr Opin HIV AIDS. 2012;7:345–53. doi:10.1097/COH.0b013e328354bd44. Silva DR, Muñoz-Torrico M, Duarte R, Galvão T, Bonini EH, Arbex FF, et al. Risk factors for tuberculosis: diabetes, smoking, alcohol use, and the use of other drugs. J Bras Pneumol. 2018;44:145–52. doi:10.1590/s1806–37562017000000443.
ʰ Lönnroth K, Williams BG, Cegielski P, Dye C. A consistent log-linear relationship between tuberculosis incidence and body mass index. Int J Epidemiol. 2010;39:149–55. doi:10.1093/ije/dyp308. Cegielski JP, McMurray DN. The relationship between malnutrition and tuberculosis: evidence from studies in humans and experimental animals. Int J Tuberc Lung Dis. 2004;8:286–98.
ᶦ Jonsson J, Kühlmann-Berenzon S, Berggren I, Bruchfeld J. Increased risk of active tuberculosis during pregnancy and postpartum: a register-based cohort study in Sweden. Eur Respir J. 2020;55:1901886. doi:10.1183/13993003.01886–2019. Sugarman J, Colvin C, Moran AC, Oxlade O. Tuberculosis in pregnancy: an estimate of the global burden of disease. Lancet Glob Health. 2014;2:e710–6. doi:10.1016/ s2214–109x(14)70330–4. doi:10.1016/S2214–109X(14)70330–4. Loto OM, Awowole I. Tuberculosis in pregnancy: a review. J Pregnancy. 2012;2012:379271. doi:10.1155/2012/379271.
ʲ Muñoz P, Rodríguez C, Bouza E. Mycobacterium tuberculosis infection in recipients of solid organ transplants. Clin Infect Dis. 2005;40:581– 7. doi:10.1086/427692. Moore DA, Lightstone L, Javid B, Friedland JS. High rates of tuberculosis in end-stage renal failure: the impact of international migration. Emerg Infect Dis. 2002;8:77–8. doi:10.3201/eid0801.010017. Moran E, Baharani J, Dedicoat M, Robinson E, Smith G, Bhomra P, et al. Risk factors associated with the development of active tuberculosis among patients with advanced chronic kidney disease. J Infect. 2018;77:291–5. doi:10.1016/j.jinf.2018.06.003.
ᵏ Uden L, Barber E, Ford N, Cooke GS. Risk of tuberculosis infection and disease for health care workers: an updated meta-analysis. Open Forum Infect Dis. 2017;4:ofx137. doi:10.1093/ofid/ofx137.
 تعليق
تعليق