Book traversal links for 1. Introduction


1.1 Background
About one fourth of the world’s population is estimated to have been infected with M. tuberculosis (1,2). The risk of TB disease after infection depends on several factors, the most important being weakened immunological status (3). The vast majority of infected individuals show no signs or symptoms of TB and are not infectious, although they are at increased risk of progressing to TB disease and becoming infectious. On average, 5–10% of those who are infected will develop TB disease during their lives, most within the first 5 years after initial infection (4). About 75% of people who develop TB disease after coming into contact with someone with TB do so within 1 year of the TB diagnosis of the index patient, and 97% develop TB within 2 years (5). Molecular typing studies in low-burden settings have also found that, among those who develop disease within 15 years of exposure, the probabilities of developing disease within 1, 2 and 5 years were 45%, 62% and 83%, respectively (6). Therefore, people living with HIV, individuals in contact with TB patients, people in congregate settings such as prisons and those with immunodeficiency conditions are at high risk of TB and are hence priority groups for receiving TPT. Unfortunately, currently available biomarkers and tests for TB infection do not differentiate between recent and past infection, and eligibility for TPT relies on ruling out TB disease clinically and radiologically among individuals and groups who are known to be at high risk of acquiring TB, with use of tests to aid decision-making, when they are available.
The WHO End TB Strategy (7) prioritizes TPT among people at high risk, as a key component of pillar 1. PMTPT fits into a larger framework of preventive action envisaged under pillars 1 and 2 of the End TB Strategy. It includes screening for TB disease, infection control, prevention and care of HIV and other comorbidities, access to universal health care, social protection and poverty alleviation. The Strategy includes indicators of progress and sets a global target of 90% coverage of TPT among people with HIV and household contacts of TB patients by 2025. PMTPT is also considered a key intervention for low TB burden countries that are pursuing TB elimination (8). While TPT services are gradually increasing globally, access by many people at risk remains low, and the targets set at the 2018 UNHLM on TB have not been met, except for the sub-target of people living with HIV. Between 2018 and 2022, 15.5 million people were provided with TPT (52% of the target of 30 million), of whom 11.3 million people had HIV (> 100% of the target), 2.2 million children under 5 years of age (55% of the target of 4 million) and 2 million people aged ≥ 5 years (10% of the target of 20 million) (9). Coverage of contacts in particular remains very low and should be a priority for scaling up.
In September 2023, at the second UNHLM on Tuberculosis, Member States endorsed a political declaration committing them to the diagnosis and treatment of 45 million people with TB by the end of 2027 and to providing 45 million individuals with TPT to protect them from developing TB disease during this period (10). The TPT target in the declaration includes 15 million people with HIV and 30 million household contacts of TB patients including children. Achievement of these targets will entail massive extension of TPT services through health system strengthening and mobilization of commensurate human and financial resources. While the investments required may be substantial, large societal returns on investment can be expected from scaling up an intensified approach to TB screening combined with TPT (Annex 1) (11,12). In this context, ministries of health should take urgent action to redesign PMTPT and mobilize resources to support rapid scaling-up of TPT, aligned with the latest (2024) guidelines from WHO (13). Table 1 lists the latest WHO recommendations on TPT, which are discussed further in this handbook.
In support of these guidelines, this operational handbook lays down key implementation considerations and steps in programmatic scaling up of TPT and provides implementation tools and job-aids for adaptation to local contexts and indicators for monitoring and evaluating PMTPT. It highlights elements to be considered in patient care, national strategic planning and resource mobilization. The handbook provides practical advice to facilitate the implementation of the evidence-based recommendations in Table 1 and does not make additional recommendations. Although the handbook focuses on settings with a high TB and HIV burden, the considerations may also apply to low TB burden settings. This handbook is intended to guide policy-makers within ministries of health and other institutions and stakeholders who are involved in health, including national, subnational and district HIV and TB programme managers; health-care workers and staff of development and technical agencies, nongovernmental organizations (NGOs) as well as civil society and community-based organizations involved in supporting TPT services.
The contents of the handbook were updated from the first edition released in 2020. The WHO secretariat oversaw the update of the text and invited experts involved in the production of the respective guidelines to review the content. (See also Annex 2 of (13)). In addition, WHO invited countries to submit examples of successful scale up of different elements of PMTPT and redacted the content to fit the style. The update of drug dosages in section 5 was developed with the input of Technical Advisory Group on dosing of TB medicines for adults and children as well as academic groups involved in the pharmacokinetic modelling of the two TPT regimens concerned. (See also Web Annex A.) Declarations of interest were sought for contributors to this handbook and were assessed by the WHO secretariat. (See also Web Annex B.)
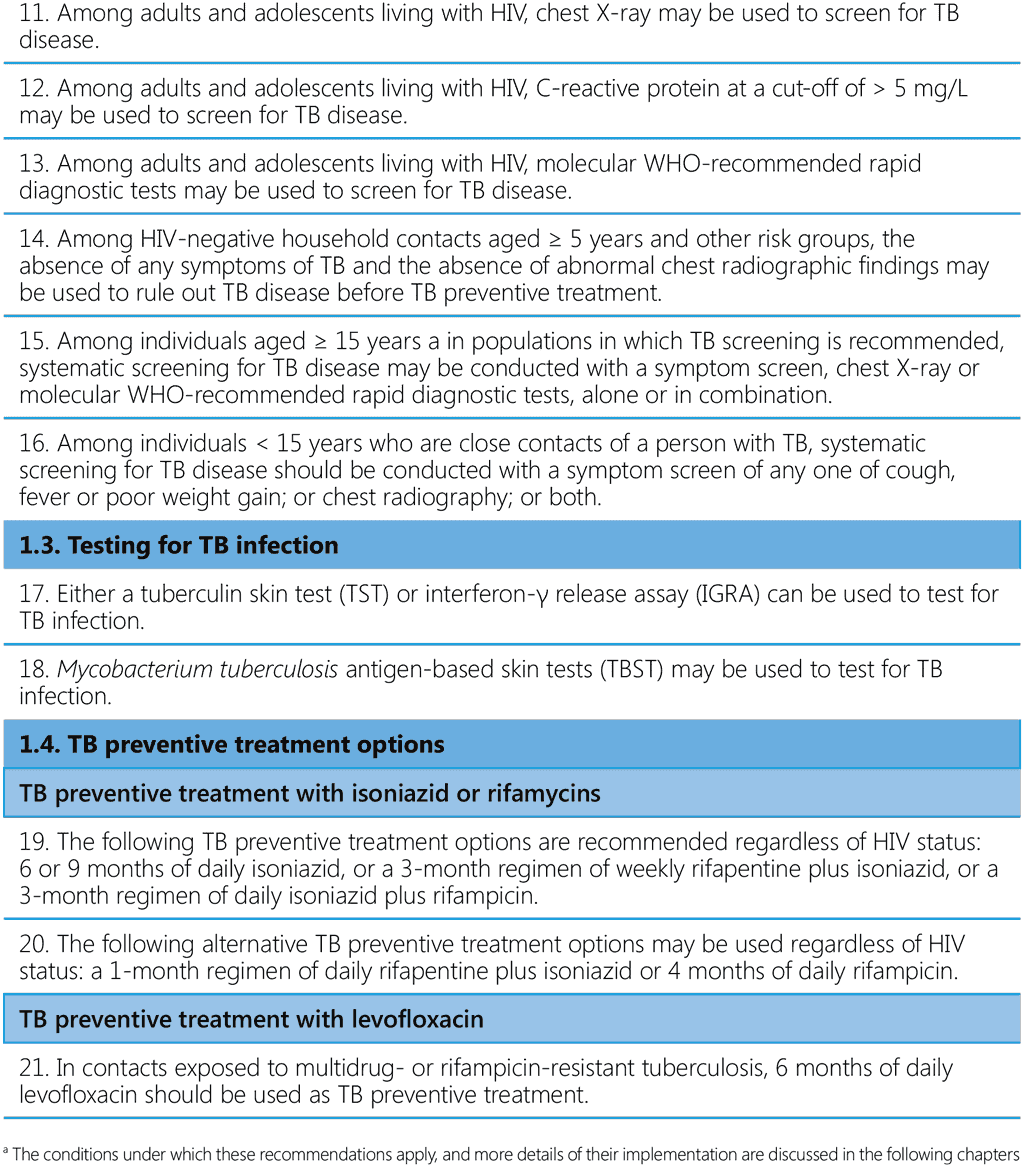
Table 1. Recommendations in the WHO consolidated guidelines on tuberculosis: tuberculosis preventive treatment (13)ᵃ

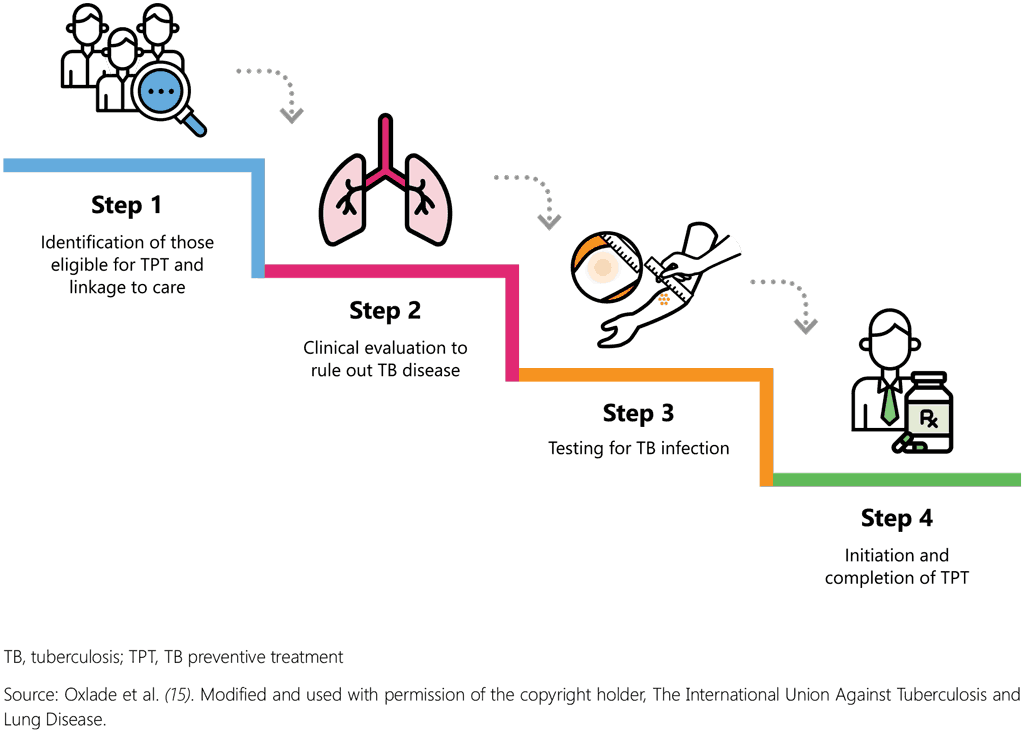
1.2 Cascade of care approach
PMTPT has long been a low-priority intervention for national programmes due to competing priorities. As Member States have committed themselves to take urgent steps to end the TB epidemic (10), however, major investments should be made in health systems strengthening and a comprehensive “cascade of care” approach adopted to scale up PMTPT (Fig. 1) (14–16). This approach for PMTPT involves four steps in which individuals move through the health system to receive care for TB infection: (i) identification of people eligible for TPT, (ii) screening for and excluding TB disease, (iii) testing for TB infection, and (iv) initiation and completion of TPT. This handbook is organized according to this cascade of care and highlights elements for programmatic prioritization and investment at each stage.
Fig. 1. Cascade of care approach to scaling TB, tuberculosis; TPT, TB preventive treatment
Programmatic implementation and scaling up of TPT services require strengthening of each element in the cascade of care, starting from identification of the target population to provision of preventive treatment (Fig. 1). This will help to ensure that individuals at greatest risk of developing TB are systematically identified, evaluated and given access to a full course of TPT to improve individual health and reduce the risk for ongoing TB transmission. A systematic review and meta-analysis have shown that there are substantial gaps in the cascade of care and that people drop out at every step, with the greatest losses at the stages of initial testing of those intended for TB screening, completing medical evaluation if the test was positive, provider recommendation of treatment and completing therapy when started (16). Overall, among those estimated to be eligible for TPT, less than 20% complete the entire cascade of care (16). It should be noted that these data are from research conducted in developed countries, and losses may be even higher under programmatic conditions in resource-constrained settings.
Annexes 2–5 present lists and other suggestions for coordinating activities in countries, costing for budgeting and planning and reviewing the PMTPT component of their health services. TPT services should be integrated into TB screening and case-finding among target populations (17). People with a positive screening result, such as symptoms of TB or abnormalities on chest radiography (CXR), should receive diagnostic testing for TB with rapid molecular tests and TB treatment if found to be positive. When TB disease is ruled out, the individual should be evaluated for TB infection and receive TPT (see also algorithm in Fig. 6 in section 4). Better retention and referral of individuals evaluated for TB, identification of those eligible for TPT and development of person-friendly, accessible services will ensure that a substantial proportion of people with TB infection are initiated on TPT and complete the treatment, thereby reducing the reservoir of TB infection from which TB disease develops (18). Advocacy at various levels is critically important. This handbook includes messages on TPT for ministries of health, health-care workers, people with HIV and other individuals offered TPT, as well as community members (Annex 2).
1.3 Components of a system for delivering TPT
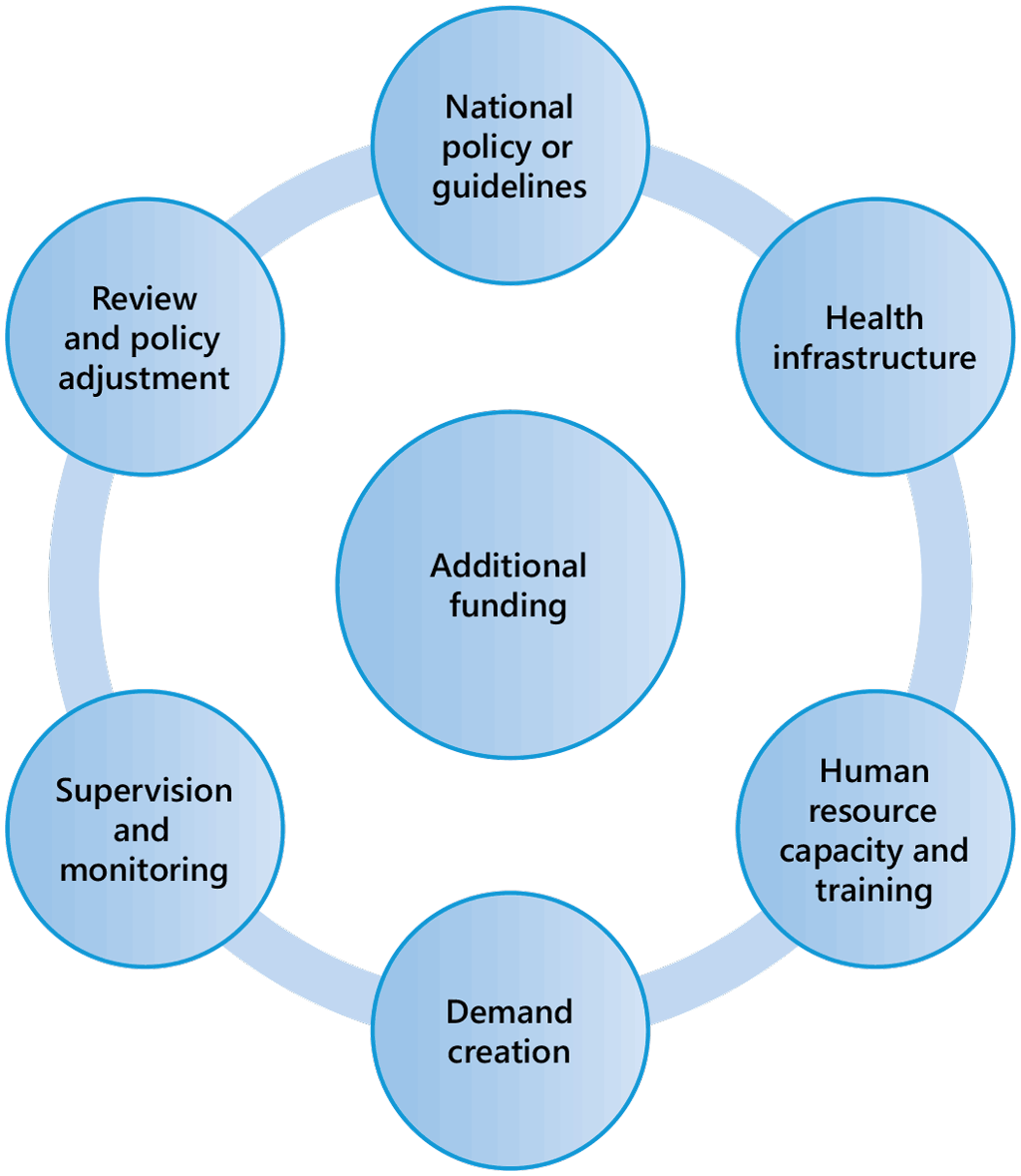
Country-specific priorities, interventions and targets should be shaped by national stakeholders according to local requirements and available resources. Fig. 2 illustrates key considerations for PMTPT.
- National policy or guidelines specify the interventions and actions to be taken by all. These should be developed through broad consultation and be based on the TPT cascade of care and the needs of at-risk populations in the framework of national TB strategic planning.
- Health infrastructure must be available to provide access to services at delivery points for TB screening, radiography, tests for TB infection and TPT. Health infrastructure includes the procurement and supply system, information technology and digital tools, and systems for community outreach.
- Human resource capacity and training are required for correct, consistent implementation of TPT guidelines. A standard curriculum and training materials and continuing education and skills-building increase the quality of the performance of care providers.
- Demand creation is essential to address the unmet need for TPT. It requires engagement of health-care providers, people eligible for TPT, people with TB and their families.
- Supervision and monitoring are indispensable for high-quality service delivery, at every level of the health system, and should complement routine monitoring, evaluation and health information activities.
- Review and policy adjustment should be conducted by a technical working group that assesses the progress of implementation and scaling-up of TPT, sets priorities for resource allocation and refines policies and practice.
- Additional funding and sustained financial investment for all components are essential for successful implementation. To ensure sustainability, TPT services could be integrated into other programmes, such as for HIV, TB case finding and methadone maintenance services. Health-care workers and communities should be adequately enabled, compensated and incentivized to scale up TPT.
Items that require costing for budgeting and planning programmatic management of TPT are listed in Annex 4. The Integrated Health Tool for planning and costing TB services is a web-based tool designed to support national strategic health planning during the medium term and can also be used for costing TPT service delivery and associated programme and health systems costs (19). Annex 5 provides a checklist (A5.1) of PMTPT components that should be considered during development of a national strategic plan and during review of national TB and/or HIV programmes.
Fig. 2. Considerations in implementing PMTPT
1.4 Objectives and structure of the operational handbook
The aim of this operational handbook is to support countries in contributing to the global targets for TPT. The policy considerations suggested are aligned with the latest WHO guidelines (Table 1). The document outlines considerations for implementation at each step in the cascade of care. Identifying and reaching populations for TPT – people with HIV and household contacts – and how to reach them are addressed in section 2, which also provides advice on establishing a system for contact investigations and integrating PMTPT into systematic screening for TB disease. Section 3 addresses the second step in the cascade of care: screening for TB and ruling out TB disease before TPT. It presents the various tools and tests that can be used to screen for TB and the stages at which they are used in the cascade of PMTPT. The third step, testing for TB infection, is addressed in section 4, including the reasons for testing for TB infection, the populations that benefit most from testing, the tests currently available, their characteristics, and arguments for and against their use. Section 5 provides an overview of the TPT regimens and dosages of TPT medication that are recommended by WHO. The section includes provision of TPT for special populations and differentiated services and implementation. Section 6 provides more details on the safety of TPT medications and on the management of adverse reactions and drug–drug interactions for people with co-morbidities who are also taking other treatments. Common questions and concerns in relation to TPT are also addressed in this section, including the duration of protection, when TPT should be repeated or reinitiated and whether TPT causes drug resistance. The importance of adherence to and completion of TPT is emphasized in section 7, which provides guidance on person-centred interventions and strategies to improve adherence, such as differentiated service delivery and nutritional support, how barriers to adherence can be addressed effectively and concrete advice on management of missed doses or interruptions of TPT. Monitoring and evaluation (M&E) are essential for PMTPT, as shown in section 8, and standard indicators for monitoring and evaluating TPT services are provided, with suggestions for data variables to be captured in a national health management information system (HMIS), preferably with digital tools to minimize the reporting burden on health-care workers. Section 9 discusses the ethics of TPT. It provides information on the requirements for obtaining informed consent and proposes ways to address issues of equity, stigmatization and human rights.
Since 2020, the WHO Global TB Programme has consolidated its normative material on all aspects of TB prevention and care into six modules: prevention, screening, diagnosis, treatment, children and adolescents and co-morbidities. The first set of guidelines and handbooks in the series was issued on World TB Day 2020, with the updated guidelines and operational handbook on TB preventive treatment, under Module 1.
In June 2021, the Global Tuberculosis Programme launched the WHO TB Knowledge Sharing Platform (TB-KSP) to enhance access to the latest WHO recommendations and resources on TB. The TB-KSP provides a “one-stop shop” for recommendations, guidelines, operational handbooks, training modules and tools to enhance research and evidence collection for policy-making, such as target product profiles. The TB-KSP may be accessed online, as an application for smartphones and tablets and on desktop and laptop computers.
The TB-KSP is constantly updated to provide users with the latest content in various languages. Users are welcome to send suggestions for continued improvement.
 Feedback
Feedback