Book traversal links for 5.2.6.1. Treatment of TB meningitis and osteoarticular TB
Following infection with M. tuberculosis, young children are at high risk of developing the most severe forms of disease, of which the most devastating is TBM. This mainly affects young children (4). Up to 15% of childhood TB presents as TBM (92). With a decreasing incidence of bacterial meningitis attributed to other causes, TB is the leading cause of bacterial meningitis in many settings (93). TBM is associated with significant mortality and morbidity. In a systematic review and meta-analysis published in 2014, the risk of death for children aged 0–14 years with TBM was estimated at 19.3%, and the risk of neurological sequelae among survivors was estimated at 36.7% (94). Even in children without severe neurological sequelae, attention deficit and behavioural disorders are common following a diagnosis of TBM and the financial burden for families and society is high. A 6-month intensive treatment regimen has been used in South Africa since 1985, with relatively favourable outcomes observed (95, 96). No relapses were observed in a subset of patients followed up for 2 years after completing treatment (95).
For the 2022 consolidated guidelines, a systematic review and meta-analysis were conducted to compare the effectiveness of the short intensive treatment regimen used in South Africa versus the current WHO-recommended 12-month regimen (6). The standard 12-month regimen, consisting of isoniazid, rifampicin, ethambutol and pyrazinamide daily for the first 2 months followed by isoniazid and rifampicin daily for an additional 10 months (2HRZE/10HR) uses doses that are the same as those for the treatment of PTB (6, 97). The recommendation on the use of the 12-month regimen was based on a literature review (98) and was first included in 2010 rapid advice: treatment of tuberculosis in children (97). The short intensive regimen is composed of daily isoniazid, rifampicin, pyrazinamide and ethionamide for 6 months throughout (6HRZEto), with higher mg/kg doses of isoniazid and rifampicin compared with the 12-month regimen (99). Ethionamide has good penetration of the blood–brain barrier (98). The 6HRZEto regimen had lower death rates and higher successful treatment rates but a higher proportion of neurological sequelae among survivors compared with the standard 12-month regimen.
The short intensive regimen is conditionally recommended as an alternative treatment option to the standard 12-month regimen (see Box 5.5). Further details can be found in the guidelines on the management of tuberculosis in children and adolescents (3).

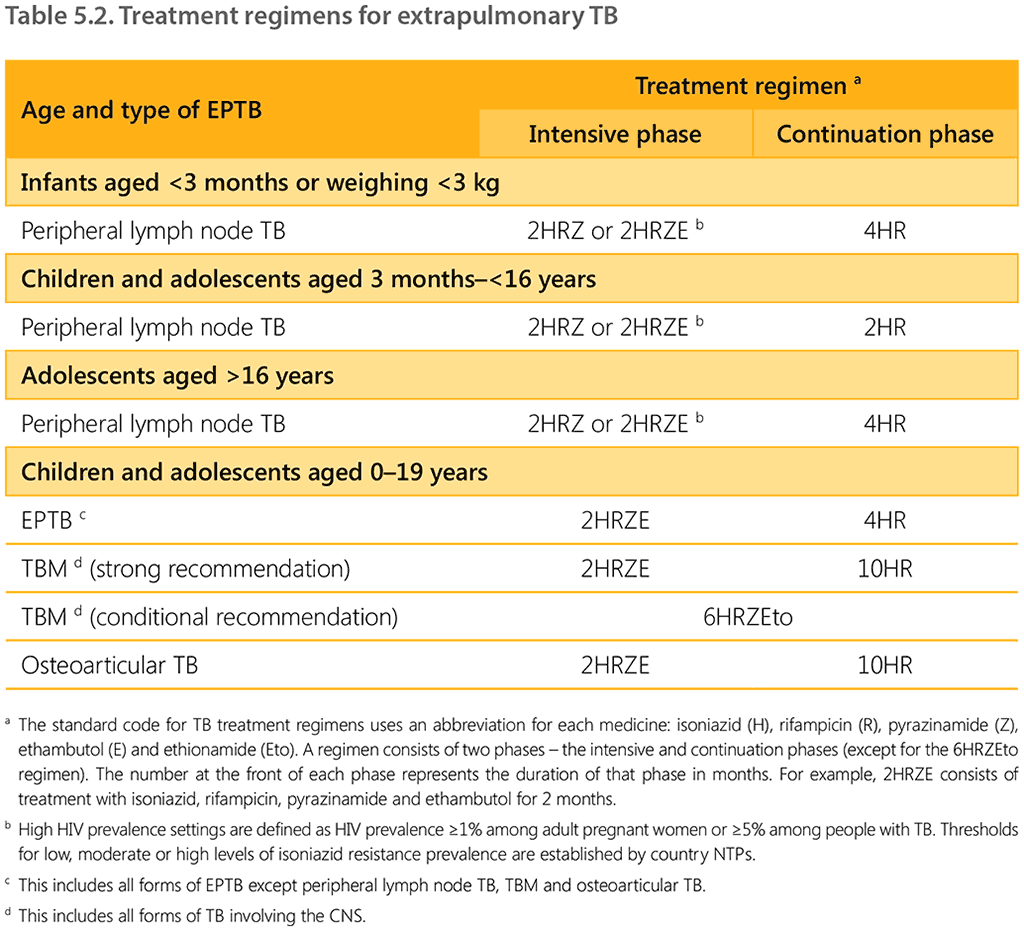
The treatment regimens for EPTB are summarized in Table 5.2.
 Feedback
Feedback