Book traversal links for 3.3.8.1. Special considerations for adherence in children
Infants and children are dependent on caregivers to administer medicines. Barriers faced by adult caregivers can contribute to children missing doses. Considerations for adherence in adolescents are covered in Section 7.4.
Potential barriers for children include the following:
- Absence of child-friendly formulations – this makes medicines more difficult to administer and increases the chances that the child will refuse treatment with crushed pills.
- Lack of conviction among the caregiver or HCW about the importance of TPT – the child’s adherence will be ensured only if the caregiver and the HCW are invested in the successful completion of TPT.
- Family factors:
- not having one or more appropriate caregivers – given that young children may move around different homes within the family, the involvement of multiple caregivers may be necessary;
- caregivers’ lack of knowledge;
- age and developmental stage at which children can be more responsible for taking their own medicines while still being supervised by an adult;
- changes in routine for the family or child (e.g. school holidays) that disrupt administration schedules;
- issues related to stigma.
Strategies for managing and enhancing adherence among children include the following (see also resources on counselling in Annex 1):
- Explain and emphasize to the caregiver and child why they must take the full course of treatment.
- For dispersible child-friendly FDCs, ensure the HCW can explain and provide clear instructions to caregivers on how to dissolve the medicine in water.
- Provide a child- and family-friendly schedule for appointments for medicine refills – for example, on the same day as other family members who are on TB treatment or TPT.
- Take note of risk factors for poor adherence and attempt to address them, such as distance to the facility, transport costs, death of a parent (especially the mother), past adverse reactions to medicines, illness in the primary caregiver, and being unwell. Address stigma through education and plain labelling of medicines.
- Provide adolescents with education and adherence support directly, especially if they are living with HIV.
- For young children refusing to take medicines:
- if taken with food, change the food type to better mask the taste, or place crushed tablets in solid food that is easy to swallow instead of mixing with water;
- provide a treat for taking the medicine completely;
- if the child vomits within 30 minutes of a dose, ensure a new dose is given. Try giving the medicine at a different time of day. Families should be given a few extra doses every month, and the programme should estimate the extent of such losses and reflect this in procurement plans. Continued vomiting requires a consultation at a health care facility.
- Prepare an adherence plan with the caregiver and ask that it be shared with other caregivers. For an example of an adherence plan, see Chapter 7 in the WHO operational handbook on tuberculosis. Module 1: prevention – tuberculosis preventive treatment (15).
- Review the adherence plan at each encounter, especially if there is a new caregiver present.
- Review knowledge and barriers at each visit. Examples of questions to ask include:
- Who is the primary caregiver?
- Does the child sometimes sleep in another family member’s home?
- Is the caregiver aware that the treatment is daily (3HR) or weekly (3HP) for 3 months?
- Is the caregiver aware of dose and pill number at each time?
- Is the caregiver being counselled regarding the need for adherence, adverse reactions, when to seek advice from a HCW, and what to do if the child vomits after taking the medicine?
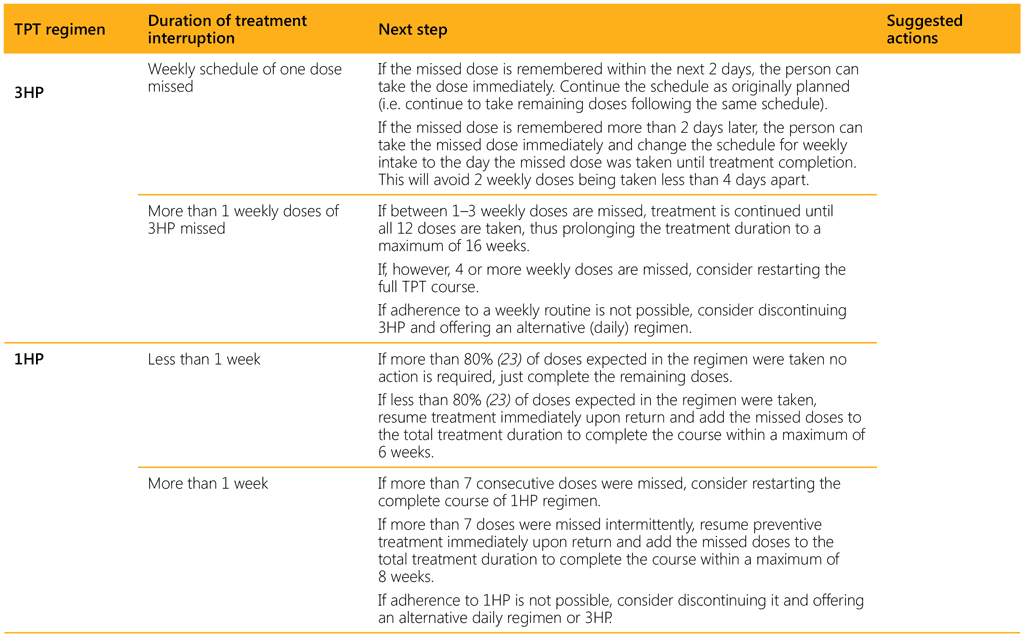
Table 3.4 summarizes all recommended regimens and suggested criteria to assess their completion. Shorter regimens are associated with better adherence and higher treatment completion, based on 80 or 90% of recommended doses taken within 133% of planned TPT duration. Table 3.5 summarizes the suggested management of interruptions in TPT.
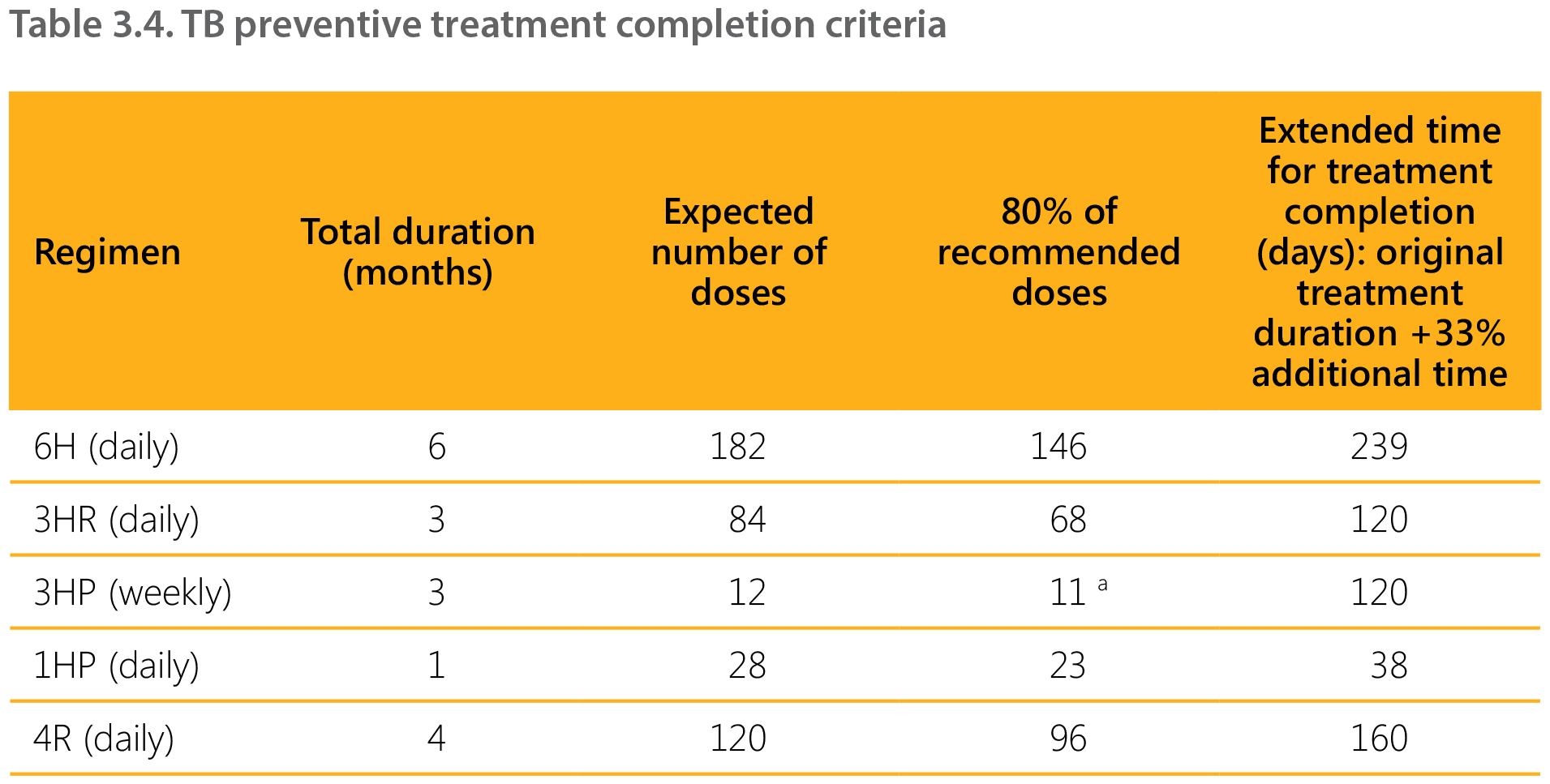
1HP: 1 month of daily isoniazid and rifapentine; 3HP: 3 months of weekly isoniazid and rifapentine; 3HR: 3 months of daily isoniazid and rifampicin; 4R: 4 months of daily rifampicin; 6H: 6 months of daily isoniazid.
a 90% of recommended number of doses for 3HP

 Feedback
Feedback