Book traversal links for 3.3.1.1 WHO-recommended four-symptom screen
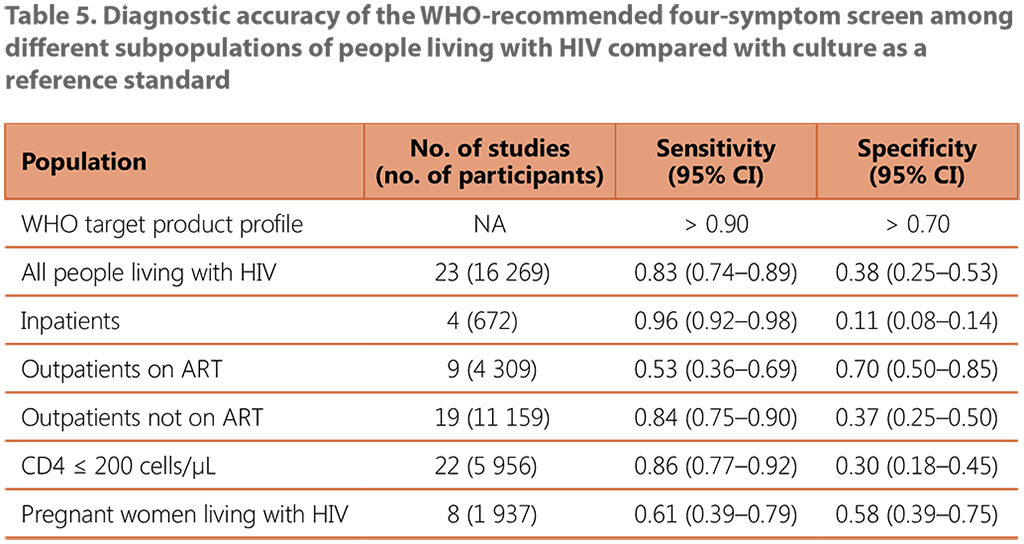
The 2020 meta-analysis of IPD included 23 studies of 16 269 participants living with HIV, all of which reviewed the accuracy of the W4SS. The studies primarily focused on pulmonary TB disease. The unweighted average TB prevalence among participants within these studies was 9.2%, ranging from 1% to 26%; and 52% of people living with HIV screened positive on the W4SS. The sensitivity of the W4SS among all people living with HIV was 83% (95% CI: 74–89) and specificity was 38% (95% CI: 25–53). Estimates of the accuracy of the W4SS in different subgroups of people living with HIV are shown in Table 5. When used alone, the W4SS was found to have its lowest sensitivity among outpatients on ART and among pregnant women, and it had markedly low specificity among medical inpatients.
While there may be real-life limitations to the W4SS in terms of consistency and quality of delivery that might not be reflected in studies, it remains the simplest non-invasive tool to implement in any setting, requiring no infrastructure. However, the high proportion of W4SS positivity (94%) and very low specificity in medical inpatients living with HIV in settings where TB prevalence among study participants was > 10% gives it limited utility as a screen to rule in TB prior to diagnostic confirmation by mWRD in this very ill population.
The meta-analysis of IPD found no alternative screening tools or strategies that were significantly higher in both sensitivity and specificity than the W4SS or that met the WHO target product profile for a screening test on both parameters. In all cases, when sensitivity was higher and met the minimal requirements of the target product profile, specificity was compromised, and vice versa. Depending on a programme’s decision to prioritize higher sensitivity or higher specificity, other tools or combinations of tools may be used to complement the W4SS.
ART: antiretroviral treatment; CI: confidence interval; NA: not applicable.
 Feedback
Feedback