Book traversal links for 3. Environmental controls
Environmental controls are the second pillar of the triad of IPC measures and should be implemented in combination with other TB IPC measures. The aim is to reduce the concentration of infectious particles in the air through a mix of interventions for dilution, removal, filtration or disinfection. In settings with a high risk of TB transmission, to protect health care workers and other individuals, WHO recommends the use of upper-room GUV systems and ventilation systems, including natural ventilation, mechanical ventilation and recirculated air through high-efficiency particulate air (HEPA) filters (Table 1.2). The evidence reviewed by the WHO GDG includes a study that showed an 8.8% reduction in TST conversion among health workers with the use of a package of interventions, including placement of upper-room GUV fixtures in patient rooms and common areas. A study using mechanical ventilation with GUV systems showed a 4.1% reduction (13), and data extrapolated from two animal studies showed a relative risk reduction of TB infection of about 72% (13). This chapter discusses GUV and ventilation systems in detail.
3.1 Upper-room GUV systems
GUV is the current term for what used to be termed “ultraviolet germicidal irradiation” (UVGI). The term “GUV” is preferred because patients and the community may wrongly associate “irradiation” with exposure to harmful ionizing radiation that may cause cancer. The effectiveness of GUV systems depends on the specifications of the GUV fixtures installed, the place of installation, quality of maintenance, the duration of exposure of contaminated air to ultraviolet (UV) light (i.e. total exposure time) and the adequacy of air mixing to ensure exposure of all infectious particles to the UV light. Upper-room GUV systems can be installed in both health facilities and congregate settings where there is a high risk of M. tuberculosis transmission. Owing to the need for capital investment, technical capacity and funding for continued maintenance, large-scale implementation of GUV systems is less feasible in low- and middle-income countries; however, implementers in such settings may prioritize locations with the highest risk of TB transmission for the installation of GUV systems.
Key point: GUV systems should be installed as part of the package of IPC interventions, not as a standalone intervention, to avoid giving a false sense of security when administrative controls and respiratory protection measures are lacking, particularly in settings with high TB transmission.
Fig. 3.1 depicts the electromagnetic spectrum of radiation (20). UV is the region of the electromagnetic spectrum from 100 to 400 nm, which is not visible to the human eye and is further split into subregions A, B and C. The visible light spectrum runs from about 400 to 700 nm whereas infrared waves may have wavelengths closer to visible light, but which are perceived more as heat. The UV light C (UVC), with wavelengths of 260–280 nm, is considered optimal for killing or inactivating most bacteria, viruses and fungi. It works by damaging DNA, RNA or proteins (20) in the microorganism and interrupting cell replication. The subregion of 200–260 nm is also germicidal but to a lesser extent and may have a better safety profile. The UVC dose required to inactivate M. tuberculosis is generally highly effective against most viruses and other bacterial pathogens; fungal spores are more UV-resistant, but they do not spread from person to person. Commercially available germicidal lamps contain mercury vapours under low pressure that emit nonionizing electromagnetic radiation in the UVC wavelength range with about 90% of the total spectral power emitted at 254 nm (UVC254). The utility of UVC254 to disinfect room air and reduce the transmission of disease has been known since the late 1930s, when it was first applied in schools to combat an epidemic of measles. Since then, much has been learned about the efficacy and safety of UVC254 to prevent M. tuberculosis transmission.
Fig. 3.1. Electromagnetic spectrum from UV to infrared radiation
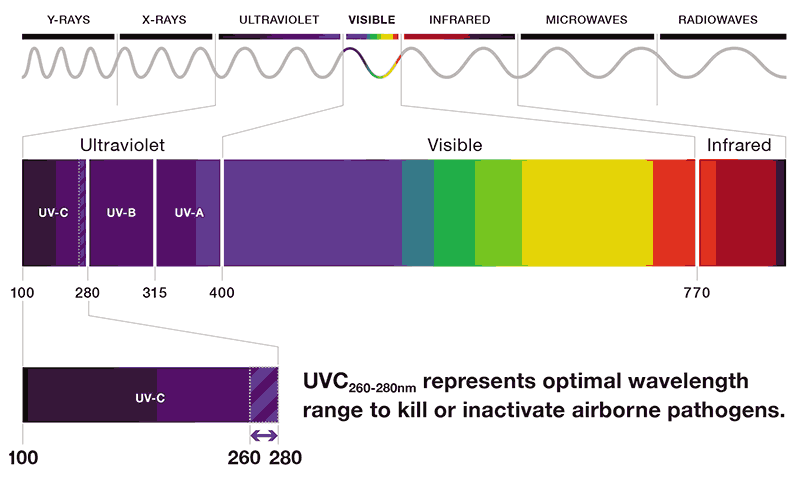
Source: Curry International Tuberculosis Center (2022) (20).
Upper-room GUV systems aim to create a disinfection zone located above the people occupying a room. They kill or inactivate any airborne pathogens that pass through the disinfection zone and thus reduce the risk of airborne infection. Upper-room GUVs can be considered an add-on to ventilation strategies in high-risk areas, particularly where unidentified infectious patients may be present. Such high-risk areas include emergency departments in hospitals, waiting rooms in busy health facilities, congregate settings or homeless shelters. GUV systems may also be suitable for:
- inpatient facilities for TB and DR-TB;
- sputum induction booths and TB treatment centres;
- isolation areas;
- facilities where natural ventilation is restricted by closed doors and windows because of cold weather; and
- spaces with insufficient or no mechanical heating, ventilation, and air conditioning (HVAC) systems.
3.1.1 GUV fixtures
Current upper-room GUV systems can disinfect the air within a space of about 40 cm from the lamp. The GUV fixture is therefore placed 40 cm from the ceiling, so that the space in between represents an area where UV radiation is effective. As with any light, the energy of UV light diminishes as the distance from the source increases. Therefore, the number of GUV fixtures required for a room depends on the size of the room. A room with GUV systems should have a ceiling that is high enough to prevent people looking into the lamp; this is shown schematically in Fig. 3.2 with a ceiling 2.5 m high, a shielded GUV device and a lamp that is oriented towards the roof. For the device to be effective, a “river” of circulating air needs to be created, to allow the “dirty” air to pass periodically through the space that has the UV radiation, to be “cleaned”
Fig. 3.2. A “river of air” facilitates movement of contaminated air for exposure to GUV
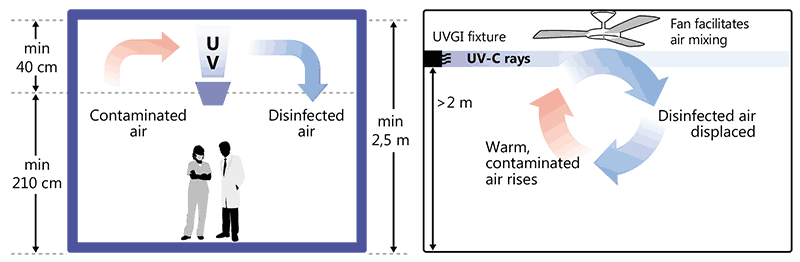
Source: images supplied by GB Migliori.
The GUV fixtures may be suspended from the ceiling or attached to the walls. The bottom of the fixture is usually shielded or louvred to direct the radiation upward above a predetermined height (Fig. 3.3). The aim is to inactivate airborne infectious agents in the upper part of the room, while minimizing the exposure to radiation of people in the lower part of the room. Panel D of Fig. 3.3 shows different types of GUV fixtures.
Fig. 3.3. Examples of GUV fixtures
Panel A. Scheme of louvreda upper-room GUV fixture and its functioningb
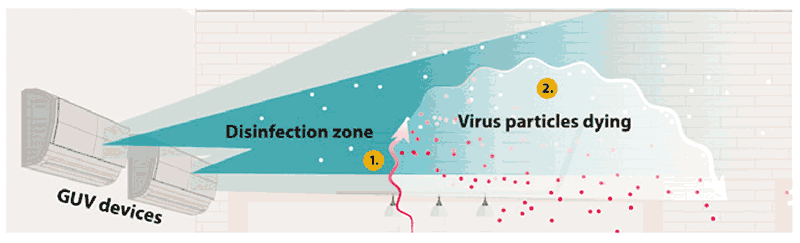
a Louvres are window blinds or shutters with horizontal slats that are angled to admit light and air.
b Air rises to the disinfection zone (Area 1) from the HVAC system, fans or open windows. The airborne pathogens are killed once they receive an appropriate amount of UVC light (Area 2). The particles remain in the air but are no longer infectious. For airborne organisms, upper-room GUV systems provide air changes per hour that are similar to the introduction of clean air into the space.
Source: US CDC (2021) (32)

Panel D. Different types of ceiling, corner and upper-room GUV fixtures

GUV: germicidal ultraviolet light; HVAC: heating, ventilation and air-conditioning; UV: ultraviolet.
Source: Stop TB Partnership (2009) (12).
Examples of GUV fixtures that are used to produce UVC wavelengths are (20):
- low-pressure mercury (Hg) lamps (emitting UVC at 254 nm);
- krypton-chloride lamps (emitting UVC at 222 nm);
- pulsed xenon lamps (emitting UVC at 220–750 nm); and
- wavelength-specific light-emitting diodes (emitting UVC at 260–280 nm).
The rest of this section discusses features of UVC254, which is the most common wavelength obtained in commercially available fixtures.
Factors influencing the effectiveness of UVC254
The effectiveness of UVC254 increases with an increase in (20):
- irradiance – the brightness or intensity of the UVC254 lamp or radiant flux per unit area, which is typically expressed in microwatts per square centimetre (µW/cm2);
- length of pathogen exposure time – the duration that the infectious particles containing a pathogen remain in the area of high irradiance; the exposure time will depend on how quickly the air containing infectious particles moves past the lamp or through the disinfection (irradiated) zone;
- dose of UVC254 – a product of the irradiance (µW/cm2) and length of exposure (seconds), expressed in microjoules per square centimetre (µJ/cm2); effectiveness and safety criteria for UVC254 are based on the dose of UVC obtained;
- output of the UVC254 fixture – relates to the UVC254 wattage (which may be a fraction of the stated lamp wattage), and the condition of the lamp and fixture; lamp intensity decreases with age and dust accumulation; also, the design of the UVC254 fixture may reduce the functional output of UVC254;
- proximity of infectious particles to the UVC254 lamp or fixture – depends on the placement and number of UVC254 lamps used; adequate mixing of the room air is needed to move infectious particles through the disinfection zone, to effectively inactivate pathogens when using upper-room UVC254 (Fig. 3.3, Panel A);
The effectiveness of UVC254 decreases with the following:
- High humidity – for optimum efficiency, relative humidity should be controlled to 60% or less (ideally at 30–60%) (13, 34–36). The effectiveness of GUV fixtures appears to reduce when the humidity in the ambient air is above 50–60% (13). More evidence is needed to determine the effectiveness of GUV fixtures above the 70% relative humidity threshold. UVC254 dosing requirements increase when the humidity of the air is greater than 70%; generally, the UVC dose will need to be increased by up to two thirds to compensate for constant humidity in this range. If high humidity is a normal occurrence, it may be necessary to install a system that has greater upper-room irradiance levels or to reduce the humidity using air-conditioning (35).
- Lower ambient temperatures – a temperature range of 20–24 °C is consistent with the optimal use of the low-pressure mercury lamps used in upper-room GUV systems. UVC254 dosing requirements increase when ambient temperatures are below 15°C.
The effectiveness of an upper-room GUV system relies on air mixing between the upper and lower parts of a room. Factors that may affect the vertical air movement and transport of the infectious microorganisms to the upper portion of the room include the temperature differential between the supply air and room air, ventilation rate and velocity of air emitted from the ventilation diffuser.
3.1.2 Considerations for the deployment of GUV systems in programmatic settings
This section outlines various factors to consider when deploying GUV systems in programmatic settings (20).
Suitability of a room for installation of GUV fixture
In determining the suitability of a room for the installation of a GUV fixture, it is important to consider architectural details as well as utilities and other engineering features in the upper room that may affect UVC coverage. For example, ceilings and walls may need to be repainted to reduce reflection and improve UVC254 safety. A room must meet the following criteria for upper-room UVC to be used:
- ceiling height at least 2.4 m – for many commercially available GUV fixtures, a minimum ceiling height of 2.6–2.7 m is recommended;
- the GUV fixtures must be installed at a height of at least 2.1–2.3 m above the floor, to ensure that people cannot look directly into the lamps or accidently bump into the fixtures;
- in rooms with lower ceilings (2.4–3.0 m), a louvred or baffled GUV fixture is needed to ensure that stray light does not overexpose occupants in the room or space; in rooms with higher ceilings (>3 m), GUV fixtures with wider spacing between the slats, or open GUV fixtures may be used;
- larger rooms or spaces may require more than one GUV fixture;
- in congregate settings, use of bunk beds should be avoided unless the rooms have very high ceilings and the GUV fixtures are placed high enough above the bunk beds to avoid overexposure; and
- fans for mixing the room air or appropriate ventilation diffusers are recommended to help increase airflow from the occupied space to the upper room and from the upper room back to the occupied space (37); the room-air fans or HVAC system fans should operate continuously while the building is occupied.
Fig. 3.4 shows which types of upper-room GUV fixtures are best, depending on the room height.
Fig. 3.4. Types of upper-room GUV fixtures best suited for different room heights
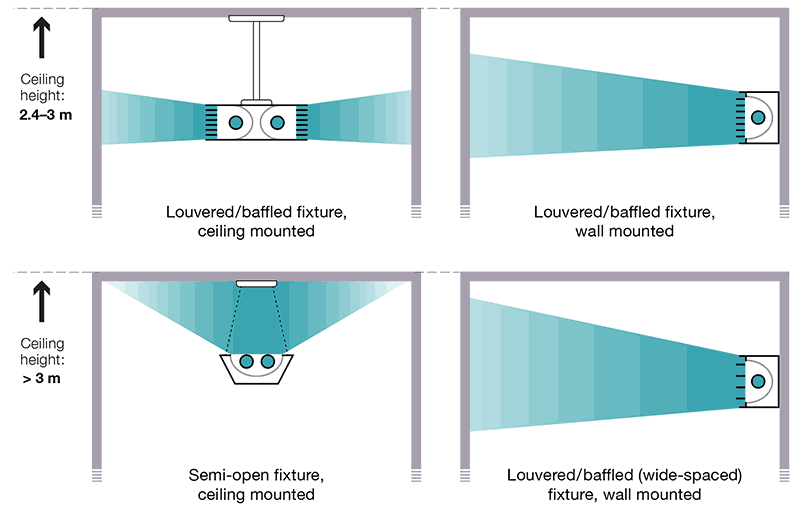
GUV: germicidal ultraviolet light.
Source: Curry International Tuberculosis Center (2022) (20)
The degree of disinfection achievable using a GUV device also depends on the UVC dose. Pathogens must either receive a dose that is sufficient to inactivate them during one pass through the disinfection zone, or they must pass through the disinfection zone multiple times until they receive a sufficient cumulative UVC dose to be inactivated.
The target UVC254 dose required to effectively disinfect for TB can be calculated using the size of the room in volume (height × width × length) or area (width × length). The volumetric dosing criterion is 12 mW/m3 and the area dosing criterion is 0.035 mW/m2 , assuming a maximum functional ceiling height of 3 m or less. A separate set of exposure dose criteria are used for the safety of room occupants.
For upper-room UVC254 systems to optimally disinfect the air, the air from the breathing zone must pass through the disinfection zone or upper room before returning to the breathing zone. Adequate “air mixing” is a key component of an upper-room GUV system design plan. Existing ventilation systems may need to be supplemented with ceiling or wall fans, or different supply-air diffusers, to accomplish adequate airflow patterns for this purpose. In the latter case, it may be necessary to keep the ventilation system fan operating at all times (i.e. constant air volume setting) during building occupancy, to ensure adequate air mixing.
The simplest way to check airflow patterns is with ventilation “smoke tubes” that can be used to show the air movement. The goal is to see the smoke moving up to the disinfection zone and back to the breathing zone in several locations. The critical criterion is the direction rather than the speed of the smoke movement.
Appropriate installation of upper-room GUV fixtures has been shown to achieve up to 24 ACH. Specialized expertise and equipment are needed to establish an effective upper room GUV system. Only a qualified contractor, working closely with the representative of a GUV fixture manufacturer, may design, install and test an upper-room UVC254 system.
Placement and number of fixtures
GUV fixtures should be placed such that radiation in the upper room is relatively uniform, continuous and complete. The number of fixtures needed to reach the target effective dose depends on the room volume (in m3), area (in m2) and shape, and the UVC254 output of the fixtures. Annex 7 has examples that illustrate how to choose GUV fixtures.
3.1.3 Exposure, safety and maintenance of upper-room GUV fixtures
Measurement of irradiance from GUV fixtures
To ensure both efficacy and safety (particularly with upper-room UVC254), irradiance should be measured and systematically recorded at the initial installation, after annual maintenance or in cases of any reported complaints or concerns related to the upper-room GUV system. The measurements and fixture maintenance should be undertaken by an industrial hygienist, health physicist, qualified engineer or technician, or a hired professional trained in measuring UV. Where feasible, training to build competency in taking measurements may also be developed within the facility. The effectiveness of GUV and the safety of fixtures are measured using a radiometer, also commonly known as a UVGI meter15 (see Annex 8). Most radiometers are programmed to display results in total irradiance.16 Radiometers take measurements to confirm the following (20):
Performance: The radiometer is used to check that the UVC254 source (the lamp) is working. The radiometer should be calibrated to measure the UVC irradiation wavelength of interest (e.g. UVC254), in accordance with the lamp manufacturers’ specifications.
Safety: The radiometer is used to check that the level of effective irradiance in the occupied areas is safe for people in the room (when using upper-room UVC254). A broad range of possible irradiation levels (0.1–2000 µW/cm2) is needed to measure both the low end of the range (to gauge safety levels in the occupied zone of a room) and the upper end of the range (to check GUV fixture performance). Proper radiometer and detector selection is critical to verify the expected irradiance levels. Depending on the type of radiometer, two separate devices may be needed to accurately obtain both sets of measurements (Annex 8).
Safety
Safety is an important consideration when using UVC254 in programmatic settings. Exposure to UVC254 radiation can occur directly or indirectly (e.g. while cleaning a fixture with the lamp turned on, or if UVC254 is unexpectedly reflected by a UV-reflective surface on the ceiling and down to occupied areas). Overexposure to UVC254 can cause temporary harm to the eyes (photokeratitis) and skin (erythema). Proper design, installation, and safety and maintenance protocols are essential to minimize the chances of overexposure (20). Systems must be monitored to ensure that optimal UV dose levels are achieved within a permissible limit of irradiance. People in the room that houses a GUV device should be shielded from excessive exposure by shields attached to the fixtures (in the form of louvres or baffles) to block the radiation and prevent it from descending below the horizontal plane of the fixture. Unshielded GUV lamps should be used only in areas that are not occupied, and the following safety features should be installed to avoid overexposure (20):
- a power cut-off switch that automatically turns the system off when a door is opened; and
- motion detectors designed to automatically turn off the fixtures when something moves above a certain height above the floor.
What level of UVC254 is safe?
Safety recommendations for UVC254 (20) are based on dose of exposure (mJ/cm2) for an individual; that is, the intensity of the radiation (irradiance, µW/cm2) from the source that reaches the individual and the duration of exposure time. There are two sets of recommendations for exposure – the recommended exposure limit (REL)17 and the threshold limit value (TLV)18 – and they are not entirely consistent:
- the REL is 6 mJ/cm2 for an 8-hour exposure for both the eyes and skin; and
- the TLV for UVC254 for eye exposure is 6 mJ/cm2 whereas for skin exposure it is 10 mJ/cm2 .
UVC254 safety education and signage
Staff and clients may have concerns about health hazards from UVC254. To address these, facilities should provide simple education on the purpose, benefits and risks associated with upper-room UVC254; for example, by:
- posting a UVC254 information sheet on the wall of the room for occupants (staff and clients);
- developing written site-specific protocols for testing, cleaning, maintenance, repair and replacement of UVC254 fixtures and providing specialized training to appropriate staff;
- ensuring that on and off switches for lamps are accessible to appropriate staff members but not located where clients may turn off the fixtures (it may be useful to consider lockable switches or placement of switches in areas restricted to staff); and
- posting warning signs, in all appropriate languages, on the GUV fixtures and other locations as appropriate (e.g. overhead storage areas), with an appropriate message, depending on the type of GUV system used (20); examples are shown in Fig. 3.5.
Fig. 3.5. Examples of appropriate wording for warning signs on UVC254 systems

Source: Curry International Tuberculosis Center (2022) (20).
Routine upkeep of GUV fixtures
One member of staff should be designated as the in-house monitor for GUV fixtures. That person should be trained in the basic principles of GUV operation and safety, and should be responsible for cleaning, maintaining and replacing the lamps, following maintenance instructions from the manufacturer.
Practical steps in routine maintenance are as follows:
- The UVC254 output should be verified. It is important to ensure that the lamps are not burned out or broken. If the tubes are working, they will emit a violet-blue glow (note: this is not an indicator of the lamp’s effectiveness, which can only be confirmed by measuring output with a calibrated radiometer).
- Dust can reduce the efficacy of GUV lamps:
- the GUV fixtures should therefore be cleaned at least once every 3 months (or more frequently, depending on local conditions);
- at least one staff member should be trained in how to clean the fixtures safely;
- before cleaning, the GUV fixtures should be turned off to avoid contact of the light with the skin and eyes and prevent heat burn;
- cleaning should be undertaken using a solution of 60–80% alcohol and a clean, soft cloth, such as a microfiber cloth; and
- the bulb and fixture should be wiped clean of dust; also, in a louvred fixture, all louvres should be cleaned (Fig. 3.6 shows a GUV device being cleaned).
- The performance of GUV fixtures should be measured 3–4 days after initial installation and then every 3 months until replacement. Before measuring the output, the fixtures should be cleaned and potential interferences (e.g. fluorescent lights or sunlight) should be blocked. Radiometers should be held 1 m away from the geometric centre of the fixture, with the face of the sensor parallel to the fixture’s louvres. Additional measurements should be taken slightly above, below, to the left and to the right of the geometric centre (Fig. 3.7).
- The irradiation level at each fixture should meet the lamp manufacturer’s recommendation. Most manufacturers will give a minimum irradiance19 (µW/cm2) value at 0.91 m from the UVC fixture, along the centreline. Lamps should be replaced once a year or as recommended by the manufacturer (or earlier if the irradiance levels are below the manufacturer’s recommended minimum levels). If a lamp has a decline of 30% or more in UV ray emission, its bulb should be replaced, even if it is still within the scheduled replacement date.
- The person performing the measurement should ensure that their eyes are protected during the process. Either UV-specific eyewear or at least clear glass or plastic eye shields should be used to block UVC.
- Radiometers should be calibrated regularly. This can be done by the supplier of the radiometer.
- A record should be kept in a logbook of all maintenance and monitoring, including radiometer readings, dates and any remedial action taken. This will help to determine the average life of the lamps. Lamps should be purchased close to the planned replacement time because prolonged storage may result in a loss of radiation intensity. Fig. 3.8 provides an example of a maintenance record.
Fig. 3.6. Cleaning a GUV fixture in a health care facility

Source: Granich et al. (1999) (10)
Fig. 3.7. Measuring the effectiveness of UVC254 and the safety of fixtures at eye level using a radiometer


Source: End TB Transmission Initiative (2017) (33). (Photo courtesy of P. Jensen).
Fig. 3.8. Example of a GUV fixture maintenance register
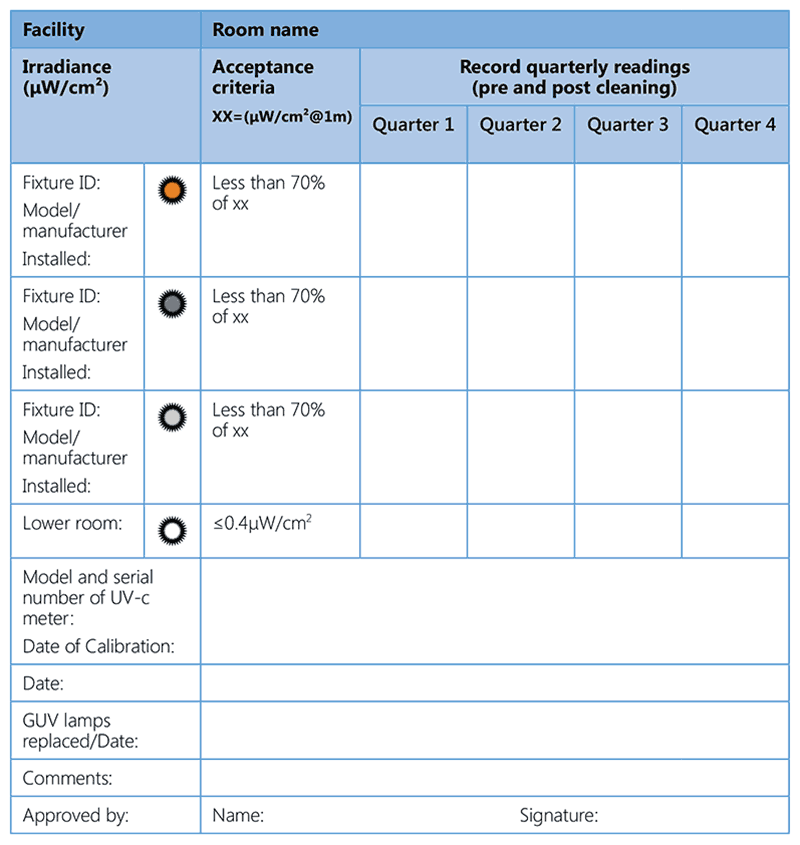
Source: End TB Transmission Initiative (2017) (33).
3.1.4 Cost considerations
Over the lifetime of a GUV system, most of the costs are typically for long-term operation and maintenance. The items listed in Table 3.1 should be considered when calculating the lifecycle cost of a GUV fixture, assuming that the “life” of a GUV fixture is 15 years.

UVC: Ultraviolet light C.
In general, the average annual cost of operating and maintaining an upper-room GUV system is 10–20% of the initial acquisition cost (38). This cost may be included as a new annual budget line for operation and maintenance at the facility level.
Key point: Upper-room GUV systems rely on effective air mixing; hence, it is necessary to ensure adequate air movement. NTPs should ensure that adequate resources are allocated for the proper installation, running and maintenance and overall sustainability of the systems.
3.2 Ventilation systems
WHO recommends the use of ventilation systems (including natural, mixed-mode, mechanical ventilation and recirculated air through HEPA filters) to reduce M. tuberculosis transmission to people in settings with a high risk of M. tuberculosis transmission. Ventilation systems, whether natural or mechanical, take advantage of air movement to push or pull infectious particles out of a space. The aim is to achieve enough air movement – as measured in terms of ACH cycles – to dilute the amount of infectious material and facilitate its removal from the room. Natural ventilation facilitates the movement of outside air into the building through doors and windows; wind pressures or the pressure gradient created by the difference in density between indoor and outdoor air determines the force of the movement. Although effective, this air movement is controlled by external environmental factors. The same effect can be achieved with mechanical ventilation systems used for air supply, air removal or both. Mechanical ventilation can also be combined with air-conditioning and filtration systems or linked with natural ventilation; this is referred to as “mixed-mode ventilation”.
There is a limited amount of evidence regarding the use and effects of standalone ventilation systems. Most of the evidence relates to mechanical and mixed-mode ventilation. The WHO GDG decided to extrapolate these data to other ventilation systems (apart from portable air cleaner appliances). All but one of the 10 studies reviewed showed reduced incidence of TB infection, with the reduction ranging from 2.9% to 11.5%. Studies reporting the use of negative-pressure isolation rooms with HEPA filtration and 20 ACH showed a reduction in TST conversion from 12–19 to 7–8 per 1000 personyears. The studies evaluating the mixed-mode ventilation also showed reductions in the rate of TB infection among health care workers.
Overall, ventilation systems are effective in diluting the concentration of particles in high-risk settings, and in effectively reducing the concentration of airborne M. tuberculosis in the air, provided the equipment is appropriately installed and functional. However, ventilation systems may actually increase airborne transmission risk if they are wrongly installed or poorly maintained. In terms of performance, the natural, mixed-mode and mechanical ventilation systems can be considered equivalent when they are well designed, installed and maintained, as shown in Fig. 3.9.
Fig. 3.9. Comparative assessment of different ventilation systemsa

a Comparative assessment using a Likert-type model for comparison of interventions through the Grading of Recommendations Assessment, Development and Evaluation (GRADE) GRADEpro Guideline Development Tool (GDT) software. All the items in this scale use the fivepoint answer format, where the lower number of qualifiers (stars) indicates the least preferred system, based on data extrapolation and on individual judgements and perceptions of each member of the Guideline Development Group on feasibility, resources required and other criteria.
Source: WHO (2019) (13).
Natural ventilation has a low cost and is simple to implement and maintain. However, it is unpredictable and not always feasible, particularly in settings with extremely hot or cold climates. Mixed-mode ventilation can overcome some of these limitations and is expected to be more affordable than fully mechanical systems, including recirculated air filtration systems. Fig. 3.10 summarizes the relative advantages and disadvantages of natural, mixed-mode and mechanical ventilation systems.
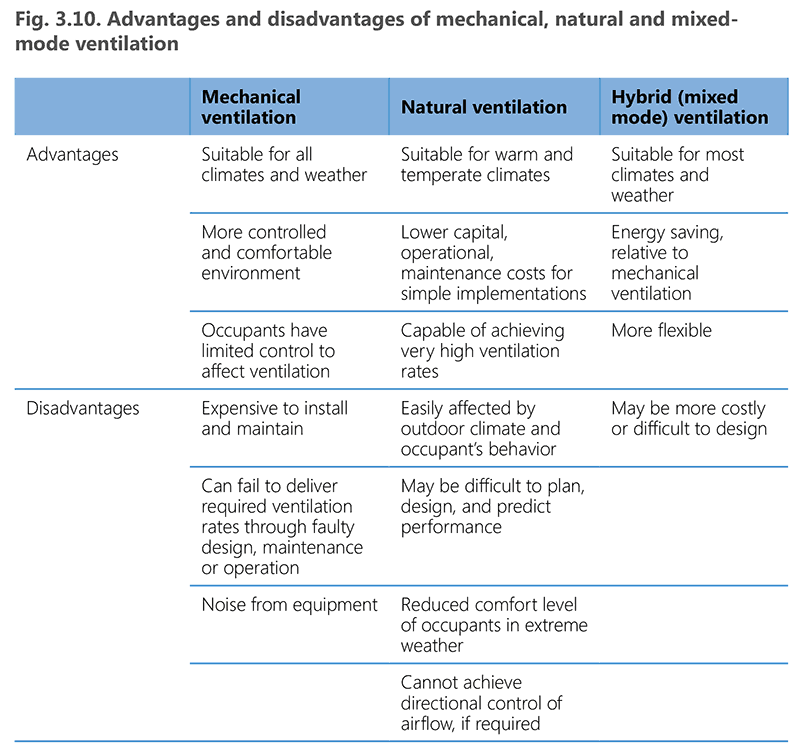
Source: Ministry of Health and Family Welfare, New Delhi (2010) (39)
Key point: A portable in-room air cleaner does not reduce the risk of TB transmission and should not be used as a TB IPC intervention.
3.2.1 Air changes per hour
Air changes per hour (ACH) is the number of times that the total air volume in a room or space is completely removed and replaced in an hour. ACH is a key consideration in determining the effectiveness of ventilation systems for the control of airborne infection. Removal of stale air and infusion of fresh air dilutes the concentration of infectious airborne organisms and reduces the risk of transmission to occupants or visitors. It is calculated by measuring the airflow rate (m3 /hour) against the volume of the room (m3). Table 3.2 summarizes the estimated time required to remove 99% or 99.9% of the infectious particles from the air by dilution ventilation if no aerosol generation takes place in a room. For example, with six ACH, it would take 46 minutes to remove 99% of the particles and 69 minutes to remove 99.9% (11, 40). With 12 ACH, it would take 23–35 minutes to remove 99–99.9% of particles, which is considered achievable and adequate. In high-transmission situations (e.g. sputum specimen collection booths) the installation of an electrical motor fan can help to achieve up to 20 ACH and allow safe use by a new patient 15–20 minutes after previous use.
Table 3.2. ACH and time required for removal efficiencies of 99% and 99.9% of airborne contaminants
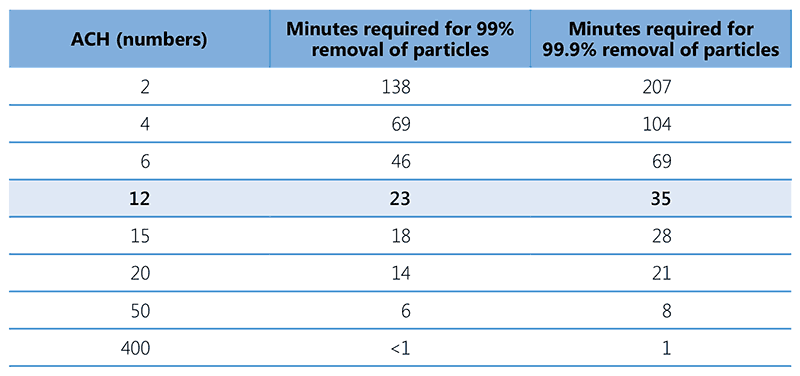
Source: Jensen et al. (2005) (40).
A vaneometer™ can be used to measure average air velocity (in m/second). Using a vane anemometer or adding a vane probe to an anemometer enables measurement of air volume flow and flow rate. A smoke tube or incense stick can be used to determine the direction of flow. Fig. 3.11 depicts the tools used to measure ACH. The measurement will also involve assessment of room volume and area of windows.
Fig. 3.11. Tools to measure ACH (including example of vaneometer with different units)

Source: image supplied by GB Migliori.
ACH measurement
The vaneometer is positioned at the level of a door or window, to measure air velocity. Multiple measurements are taken at different levels – ideally, three measurements each at the top, middle and lower third of the window or door opening – to compute an average air velocity (in m/second). Fig. 3.12 provides an example of an ACH measurement in a room with two beds, two closed windows, two open windows and a door. It shows the dimensions of the room (4.5 m × 4.0 m × 3.5 m) and the open windows (1 m × 1 m), as well as the related air velocities (0.2 m/s and 0.1 m/s), as measured with a vaneometer. The diagram and the box to its right in Fig. 3.12 depict the steps used to calculate ACH for this room, which are as follows:
- Step 1. Calculate the room volume.
- Step 2. Calculate the area of the open windows.
- Step 3. Measure the air velocity using the vaneometer and calculate the average air velocity using the three readings per window.
- Step 4. Multiply the average air velocity by the area of the windows and the measure of time (i.e. 3600 seconds) to obtain the average flow rate per hour
- Step 5. Determine the ACH required to clean the air in this room by dividing the average flow rate per hour by the volume of the room. The required ACH is 17.14 in the example shown in Fig. 3.12.
Fig. 3.12. Steps for calculating ACH for a room
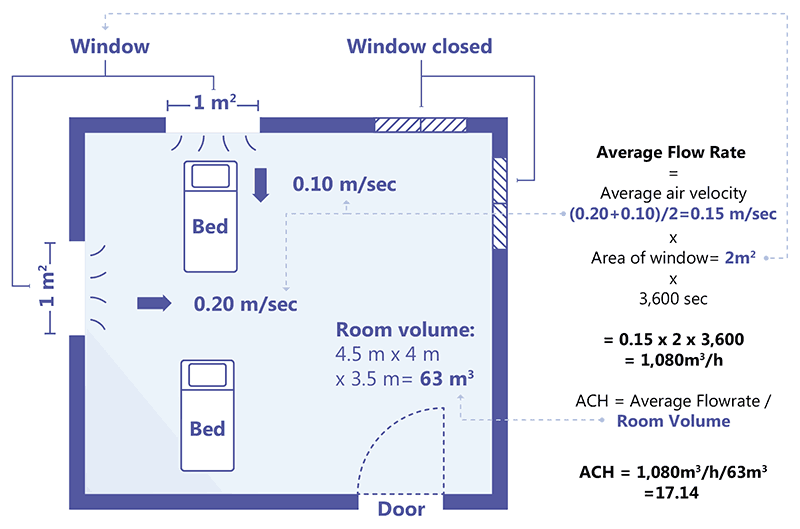
Source: image supplied by GB Migliori
Choice of ventilation system
The decision on which ventilation system to use (i.e. natural, mechanical, mixed-mode ventilation or recirculated air with HEPA filtration) depends on the IPC needs in a particular setting; that is, level of risk of TB transmission, weather, cost-effectiveness and sustainability (Fig. 3.9 and Fig. 3.10). Installing poorly designed ventilation systems, or failing to maintain ventilation systems, produces results contrary to those intended and may cause health care-associated transmission of M. tuberculosis. Such suboptimal ventilation systems also increase risks in congregate settings. The subsections below discuss the different ventilation systems.
3.2.2 Natural ventilation
Natural ventilation is achieved with natural airflow caused by the temperature differential between spaces or by a wind-driven pressure differential. As the air warms, its density lowers and it rises to the upper part of a space, towards a chimney, tower or windows. Such differences in air density create a gradient within the room or between the interior and exterior air columns, causing a vertical pressure difference. When the room air is warmer than the outside air, the room air is less dense; hence, it rises and escapes from outlets around the roof. Cooler air then enters the building through lower openings, heats up and rises to escape from openings at the upper level, creating a cycle. This phenomenon, which occurs because of the natural heat transfer, is called a stack effect or a chimney effect Fig. 3.13. The possibility of stack ventilation should be considered during the construction of a building (41) because it generates passive cooling during summers. The airflow direction may sometimes (albeit rarely) reverse when the room air is cooler or denser than the outside air; in such cases, air may enter through upper openings and escape through lower openings. Natural ventilation does not need any electricity and can work 24 hours a day without maintenance or running costs. Naturally ventilated rooms can achieve a high rate of ACH. However, changes in wind direction or temperature can affect the airflow rate, and climate strongly influences the quality of ventilation. On a windy or rainy day, there may be excessive ventilation, much more humidity and greater air velocity, creating a need for airflow control using dampers or shutters. Nevertheless, natural ventilation may be preferred in resource-limited settings that may lack capital investment, uninterrupted availability of electricity and skilled staff to maintain complex mechanical systems.
Fig. 3.13. Stack ventilation
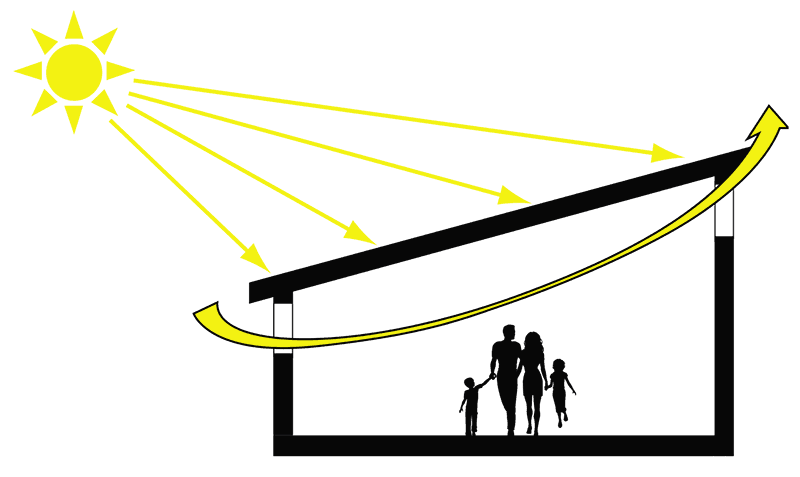
Source: Stop TB Partnership (2009) (12)
To achieve optimum ventilation and ACH with natural ventilation, it is necessary to ensure that:
- the area of doors and windows that can open constitutes more than 20% of the floor area (e.g. a room of 10 m2 should have fixed, unrestricted openings of about 1 m2 on two sites, giving a total of 2 m2 of openings);
- there are openings on opposite walls for cross-ventilation;
- openings are unrestricted (e.g. doors and windows are kept open during patient visits); and
- upper levels of the building are better ventilated than lower levels.
Wind direction and the airflow rate should be considered when deciding on the seating arrangements for the patients and health care workers in consultation rooms. Fig. 3.14 depicts a consultation room with the seating arrangements to use or avoid, based on the airflow direction. The officer in charge of the health facility should ensure that health care workers are closest to the source of clean air and patients are closest to the point of air exhaust, to ensure that contaminated air does not blow towards the health care worker. The seating arrangement should be decided on after repeated observations and measurements at different times of the day (e.g. sunrise vs sunset) and in different seasons (e.g. hot and humid summer vs cold and dry winter).
Fig. 3.14. Incorrect, correct and neutral ways to locate the seating for health care workers and patients in a consultation room with natural ventilation (12)
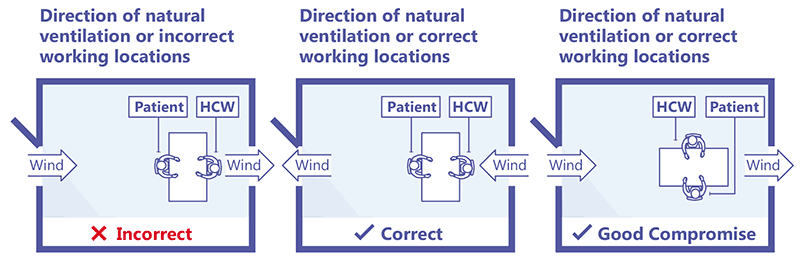
HCW: health care worker
Source: Stop TB Partnership (2009) (12).
Fig. 3.15 shows an example of a natural ventilation system in a TB referral hospital in Peru (41) and
Fig. 3.16 shows a naturally ventilated health centre in South Africa.
Fig. 3.15. Layout of natural ventilation system, Hospital Nacional Dos de Mayo, Fig. 3.15 Lima, Peru
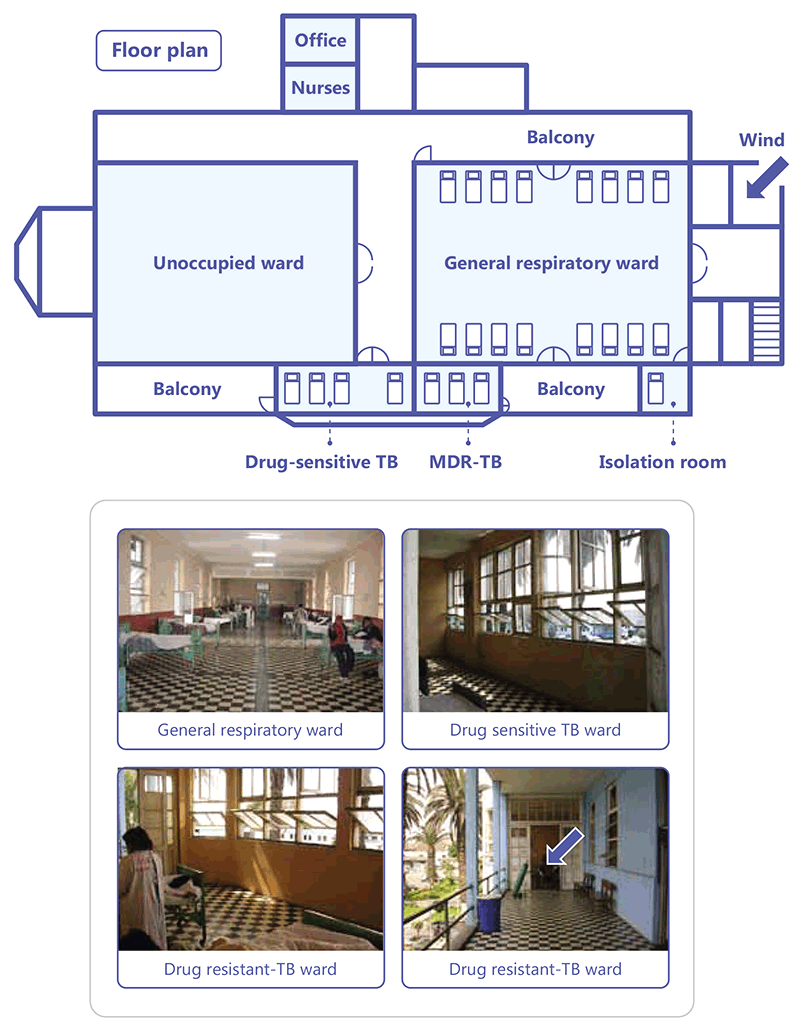
Source: WHO (2009) (41).
Fig. 3.16. Example of natural ventilation at a health centre in South Africa

Source: Curry International Tuberculosis Center (2022) (20).
The floor plan in Fig. 3.15 shows that the ward for patients with DS-TB, with four beds, is well ventilated, given the high ratio of window and door area to the room volume, despite this ward being on the side of the building protected from prevailing winds. The MDR-TB ward has three beds and is adjacent to the DS-TB ward; however, it has separate access and its exposure to the prevailing winds is similar to that of the DS-TB ward. Smoke tube testing consistently demonstrated airflow in through the door and out through the windows. The isolation room is located off the main general respiratory ward. The door connects with the general respiratory ward, and three windows open to the outside. With the door closed, a mean of 23 ACH was measured with all three windows fully open. Opening the door produces cross ventilation and increased the mean to up to 49 ACH. Smoke testing consistently demonstrated that the direction of airflow was from the main ward into the isolation room and out of the windows.
Often, the waiting area in hospitals and clinics is poorly ventilated, increasing the risk of M. tuberculosis transmission for both health care workers and visitors. Fig. 3.17 depicts an example of a hospital in Peru where renovation in the outpatient department helped to significantly reduce this risk. In the plan, the waiting area is located next to various consulting rooms (medical specialities, surgery and psychiatry). A front entrance leads in from the street, and doors at the other end lead into different parts of the hospital. On a typical day, up to 300 patients share the waiting space during the consulting hours. Originally, the roof in this space was sealed with four glass sections, two measuring 14 m × 2.4 m and two measuring 5 m × 2.4 m. The renovation involved raising the height of these sealed sections by 1 m, with openings allowing air entry into the waiting room (as shown by the arrow in picture 2 of Fig. 3.17). This improved the natural ventilation from about 6.5 to 15 ACH. Structural changes were also made from outside the building and some windows were converted into doors, creating additional air entry into the consulting rooms (the bottom right panel in Fig. 3.17). The waiting area was shifted outside with a simple covered roof for shade. This combination of measures helped to improve ventilation in the health facility and reduce the risk of infection transmission (10).
Fig. 3.17. Improving natural ventilation in an outpatient clinic
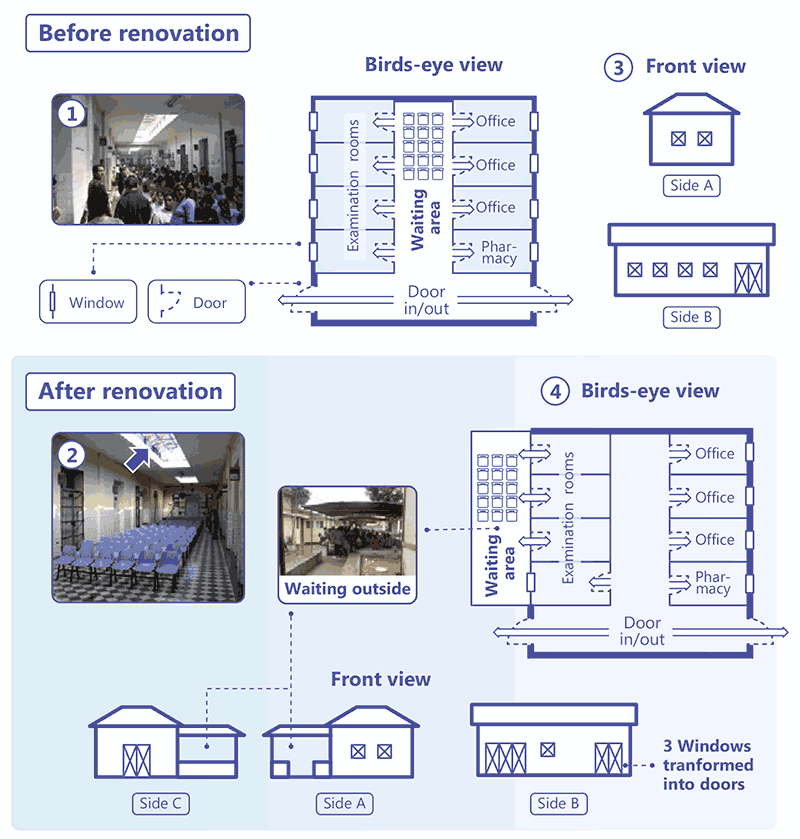
Source: image supplied by GB Migliori.
The photos in Fig. 3.18 present good examples of well-ventilated waiting spaces in and around health facilities.
Fig.3.18. Examples of natural ventilation in the waiting areas of four outpatient clinics

3.2.3 Mechanical ventilation
The use of mechanical ventilation, mixed-mode ventilation or HEPA filters may be feasible in settings where resources are available, or where natural ventilation is not suitable or is unreliable owing to the weather. Mechanical ventilation works by creating negative pressure (Fig. 3.19), which draws in air from higher pressure areas and uses the pressure gradient to create airflow between different rooms. The system is designed to enable air to move from “clean” areas to “dirty” areas.
Fig. 3.19. Air pressure gradient with mechanical ventilation
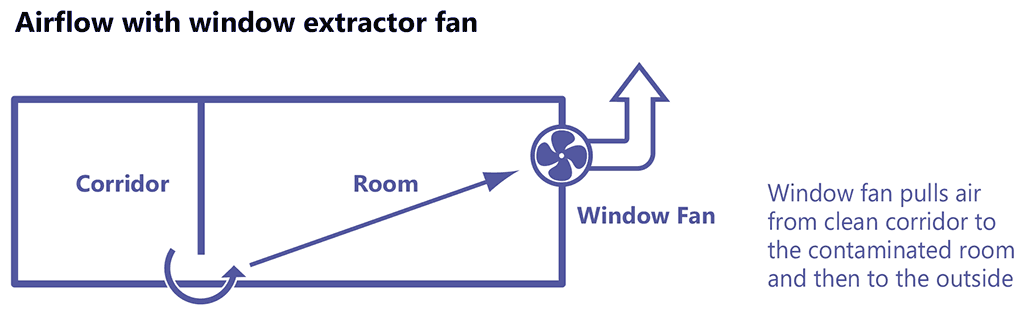
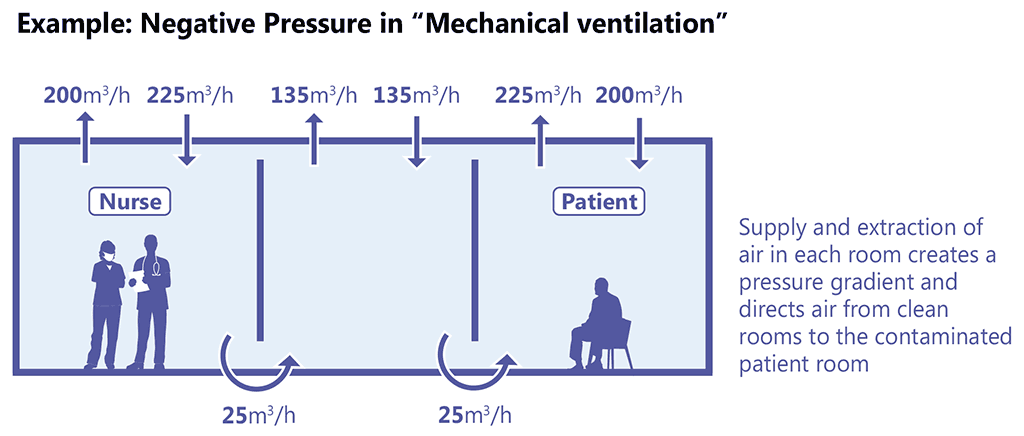
Source: Stop TB Partnership (2009) (12).
Airflow patterns are affected by the temperature and configuration of the space, and by physical barriers to airflow, such as furniture. The diagrams on the left in Fig. 3.20 show two scenarios with appropriate location of the source of clean air supply and the exhaust, which allows for good air mixing. Conversely, the diagram on the right presents a scenario where the air supply and the exhaust are located in such a way that the clean air is removed before it can mix with the potentially contaminated air, thus prohibiting dilution of the contaminated air.
Fig. 3.20. Layout of rooms with good and suboptimal air mixing
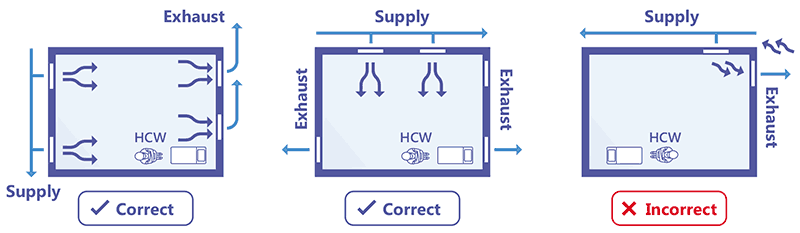
Source: Jensen et al. (2005) (40)
Sometimes, poor engineering design can increase the risk of contamination or produce short-circuiting, as shown in Fig. 3.21. In this example, the position of the exhaust air fan increases the likelihood of contaminated air being reintroduced through the supply inlet. Such short-circuiting can be avoided if the supply inlet is located at least 10 m away from the exhaust.
Fig. 3.21. Short-circuiting in a mechanical ventilation system, causing contaminated air to be recirculated

Source: image supplied by GB Migliori.
Mechanical ventilation can also be ensured through an entirely closed system (Fig. 3.22), where air is recirculated and filtered using special filters (e.g. HEPA filters), and filtered air is reintroduced into the facility. In closed mechanical ventilation systems, maintenance of the HEPA filters is paramount because dirty filters can modify the airflow and reduce effectiveness. Mechanical ventilation systems should be professionally designed, installed and maintained, to allow good mixing of air and dilution of contaminated air, although this is usually costly.
Fig. 3.22. Example of mechanical ventilation equipment

MDR-TB ward, Radboud University Medical Centre, The Netherlands.
Source: Stop TB Partnership (2009) (12).
3.2.4 HEPA filters
HEPA filters can be used as part of mechanical ventilation systems to filter out infectious particles from recycled air, or as part of a compact in-room-air cleaner. They should always be considered as an adjunct to other ventilation measures; used alone, they do not provide outside air for the occupant’s comfort, nor do they enhance ventilation.
HEPA filters are composed of a mesh of randomly arranged fibres. The fibres typically comprise polypropylene or fibreglass with diameters of 0.5–2.0 µm. Often, these filters are tangled bundles of fine fibres that create a narrow, winding pathway through which air passes. When the largest particles are passing through this pathway, the bundles of fibres behave like a sieve and physically block the particles from passing through. However, when smaller particles pass through the pathway, as the air twists and turns, they cannot keep up with the air’s motion and they collide with the fibres. The smallest particles have little inertia and move around the air molecules as they are bombarded by these molecules. Because of their movement, the smaller particles also end up crashing into the fibres. Key factors affecting filter functions are the fibres’ diameter, the filter thickness and the face velocity; that is, the rate of air movement at the face of the air filter (airflow rate divided by face area). The air space between HEPA filter fibres is typically much greater than 0.3 μm. However, the design is such that a range of particle sizes are trapped through a combination of the following mechanisms:
- diffusion – particles below 0.3 μm in size are captured by diffusion resulting from the collision of the smallest particles with air molecules; the small particles are effectively blown or bounced around and collide with the filter fibres;
- interception – mid-size particles are intercepted when they are in a line of flow with the air stream and come within one radius of a fibre and adhere to it; and
- impaction – larger particles are unable to avoid fibres by following the curving contours of the airstream and are forced to embed directly in a fibre.
The HEPA filters can be used to clean air before it is extracted from a room to the outside via an exhaust fan, recirculated to other areas in a health care facility, or recirculated into an airborne infection control or negative-pressure room. To ensure adequate functioning, HEPA filters should be installed carefully, and the filters should be maintained in accordance with the manufacturer’s instructions. Improper design, installation or maintenance of HEPA filters can allow infectious particles to circumvent filtration and escape into the general ventilation system. A manometer or other pressure-sensing device should be installed in the filter system to provide an accurate and objective way to determine the need for filter replacement. The filters can also degrade over time with exposure to humidity and ambient aerosols; hence, in general they should not be used in systems that recirculate air back into the general ventilation system from negative-pressure rooms and treatment rooms. If filters are used in that way, the filter manufacturer should be consulted regarding the performance of the filter, to ensure that it maintains the desired filtration efficiency over time. There should be written records of all HEPA filter maintenance and monitoring (42).
3.2.5 Mixed-mode ventilation
Ventilation systems that combine the use of mechanical and natural ventilation are called hybrid or mixed-mode systems. Propeller fans may be used to increase air circulation, along with exhaust fans, to generate areas of negative air pressure that will draw in air. This may increase air movement from the outside, enhancing ACH in the room when the system is appropriately designed. Such systems can be designed where natural ventilation is not suitable (e.g. owing to very cold weather) or fully mechanical ventilation is not available. Evaporative coolers or desert coolers may be an effective solution in hot weather to achieve both comfort and adequate ventilation. In cold weather, doors and windows may need to be closed; hence, high ventilation rates are difficult to achieve and air exhaust fans may be needed to enhance ventilation. Propeller fans placed on a desk, floor or ceiling may not be able to ensure an adequate supply of fresh air or to expel room air to the outdoors, to achieve the required number amount of ACH. Regular measurements of ACH should guide the choice of equipment and its placement to enhance ventilation.
In scenarios where there is only one window and that window may need to be closed, the amount of air entering the room is curtailed. In such situations, turbines could be used as the exhaust system and to enhance natural ventilation (Fig. 3.23).
Fig. 3.23. Turbine-driven natural ventilation
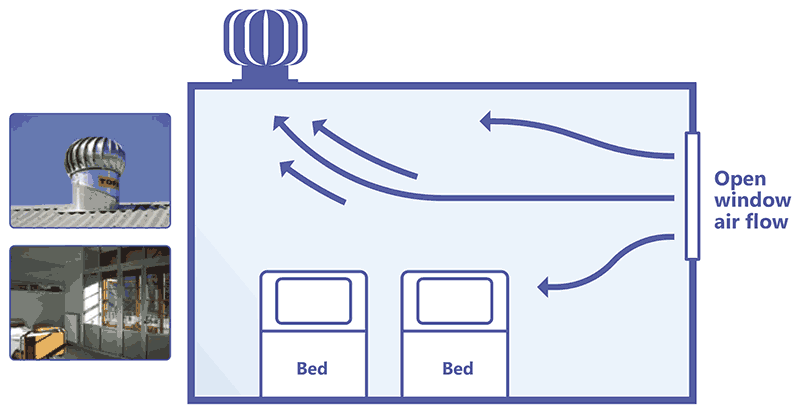
Source: image supplied by GB Migliori and Paul Jensen
Key point: Given the cost and the high risk of design or maintenance failures, ventilation systems that recirculate air may not be suitable for settings with a high risk of M. tuberculosis transmission, such as TB inpatient wards. In such settings, natural or hybrid mechanical ventilation without recirculation or upper-room GUV systems may be more suitable.
15 Examples of devices used to monitor UV dose levels include the International Light meter model 1400A with SEL240 detector and the Gigahertz-Optik X1–1-UV-3718 UVC radiometer.
16 The actual irradiance at each wavelength is referred to as the spectral irradiance. The total irradiance (for photobiologic activity) at each wavelength can vary and differs from the measured effective irradiance (except at 270 nm, where they are the same). Most radiometers are programmed to display results in total irradiance rather than effective irradiance. The relationship between effective irradiance and spectral irradiance for each wavelength requires a conversion factor. For UVC254, multiplying the total irradiance by 2 gives the effective irradiance.
17 CDC/National Institute for Occupational Safety and Health (CDC/NIOSH), USA, Recommended exposure limit for GUV energy at the UVC254 wavelength published in 1973.
18 The American Conference of Governmental Industrial Hygienists (ACGIH) updated the TLV for ultraviolet radiation and designated separate values for eye exposure and for skin exposure by wavelength in 2022.
19 Most manufacturers give irradiance based on effective irradiance; however, most UVC254 radiometers measure total irradiance, and total irradiance results should be multiplied by 2 (conversion factor to effective irradiance).
 Feedback
Feedback