Book traversal links for 4.4 Diagnostic approaches: extrapulmonary TB
EPTB refers to any bacteriologically confirmed or clinically diagnosed case of TB involving organs other than the lungs (e.g. pleura, peripheral lymph nodes, abdomen, genitourinary tract, skin, joints and bones, meninges) (71). The classification of intrathoracic lymphadenopathy in children was updated following an expert consultation in September 2021 as PTB. EPTB is common in young children and in children and adolescents living with HIV. Since it is more difficult to diagnose, children with presumed EPTB, especially those who are very ill, should be urgently evaluated or referred for further evaluation and diagnostic workup (see Table 4.6). Symptoms of EPTB vary, depending on the site of disease. They are usually persistent and progressive and may be associated with weight loss, poor weight gain and fever.
Clinical assessment in all presumed cases of EPTB should consider:
- history of TB contact (as above);
- collection of appropriate specimens from an affected site (including CSF, lymph node aspirate, lymph node biopsy, pleural fluid, peritoneal fluid, pericardial fluid, synovial fluid or urine specimens) for confirmatory tests, including mWRDs (and histology where appropriate and available);
- collection of respiratory samples (stool, expectorated or induced sputum, gastric aspirate or NPA sample) to evaluate for PTB (as the child may have both PTB and EPTB);
- CXR and other imaging, depending on the affected site;
- HIV testing.

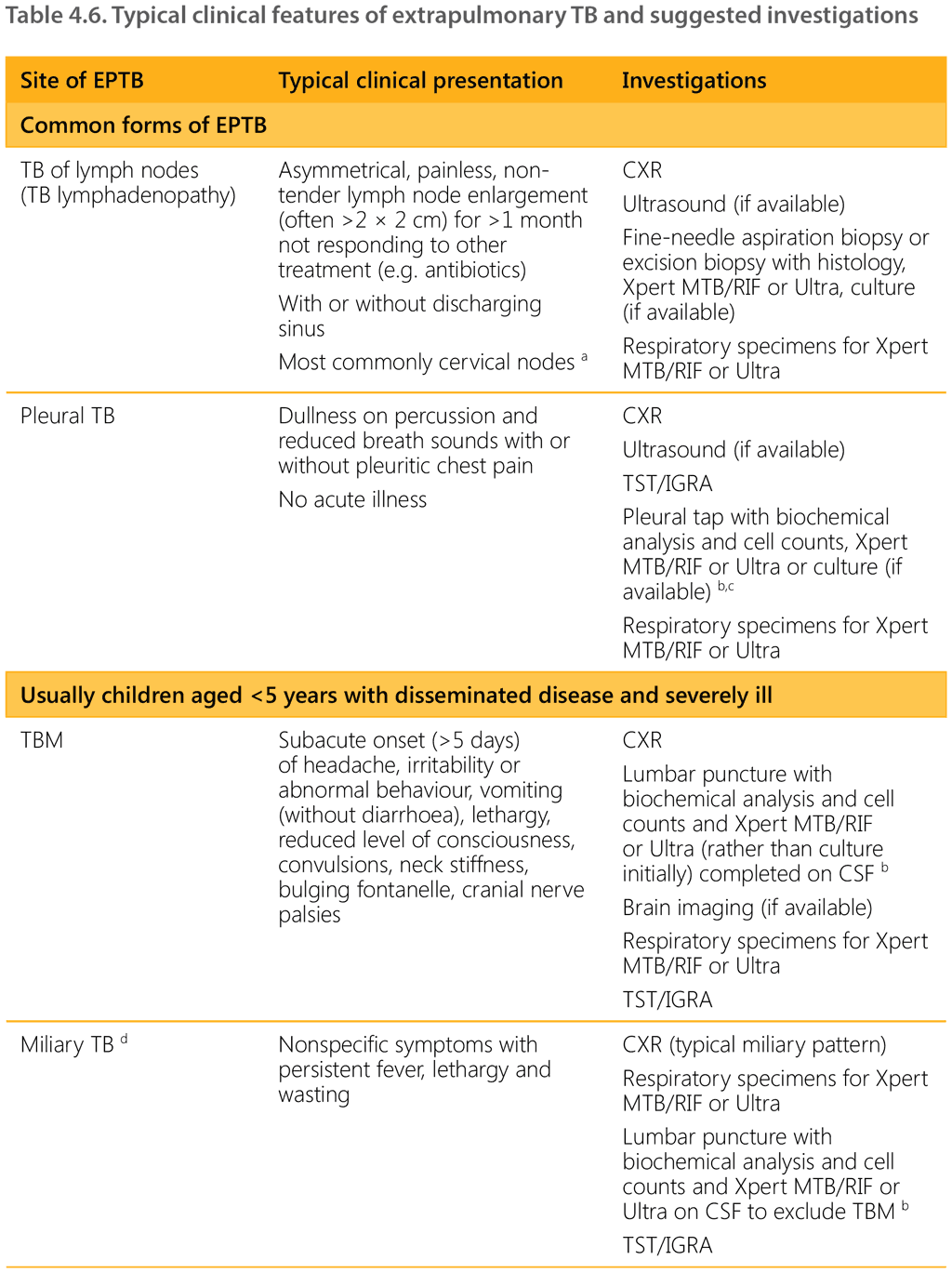
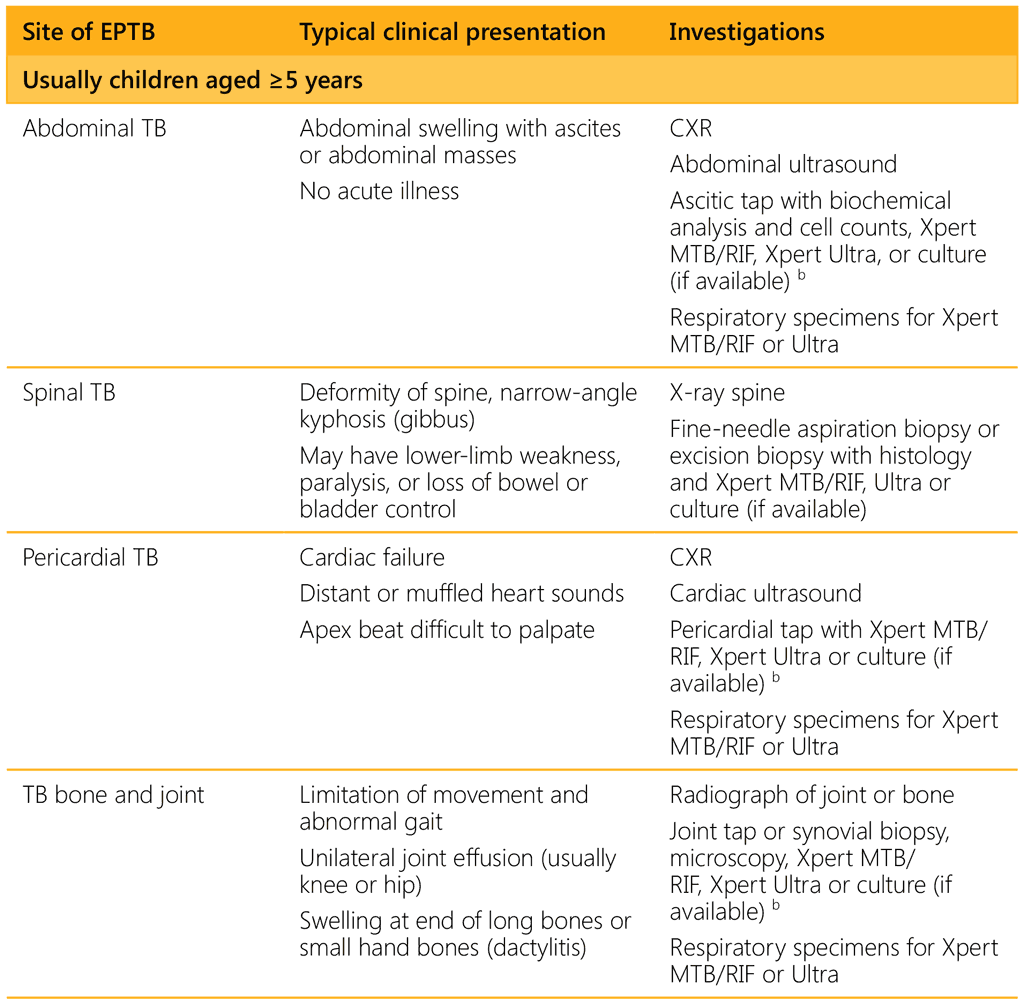
a If axillary node enlargement on same side as BCG vaccination, consider BCG disease.
b Typical findings suggesting TB on effusions (straw-coloured fluid, exudate with high protein, white blood cells (typically predominance of
lymphocytes) on microscopy, positive Xpert MTB/RIF, Xpert Ultra or culture) or CSF (high protein, low glucose, white blood cells (typically
predominance of lymphocytes) on microscopy, positive Xpert MTB/RIF, Xpert Ultra or culture).
c If pus in tap, consider empyema.
d Miliary TB is classified as PTB but often involves extrapulmonary features that can occur anywhere in the body.
Source: adapted from Guidance for national tuberculosis programmes on the management of tuberculosis in children, second edition. Geneva: World Health Organization; 2014 (https://apps.who.int/iris/rest/bitstreams/514493/retrieve) (6); and The Union’s desk guide for diagnosis and management of TB in children, third edition. Paris: International Union Against Tuberculosis and Lung Disease; 2016 (https://theunion.org/sites/default/files/2020–08/2016_Desk-guide_Africa_Web.pdf) (72).
 Feedback
Feedback