Book traversal links for 1.3 Objectives of the operational handbook
This document provides practical guidance on translating WHO’s recommendations for screening into a national or local strategy with clear objectives, prioritization of risk groups and definition of the most appropriate screening approaches.
The specific objectives are:
- to support Member States in implementing effective TB screening by supporting policymakers in ministries of health in choosing the best approach to planning and implementing screening and active case-finding, depending on the context;
- to provide a sound basis for development or updating of national guidelines for TB screening according to the epidemiology of TB in different risk groups and the health care delivery system in the country; and
- to contribute to finding people with TB who may be missed by standard case-finding approaches and finding people with TB earlier in the course of disease to reduce transmission, morbidity, mortality and financial hardship for people suffering from TB.
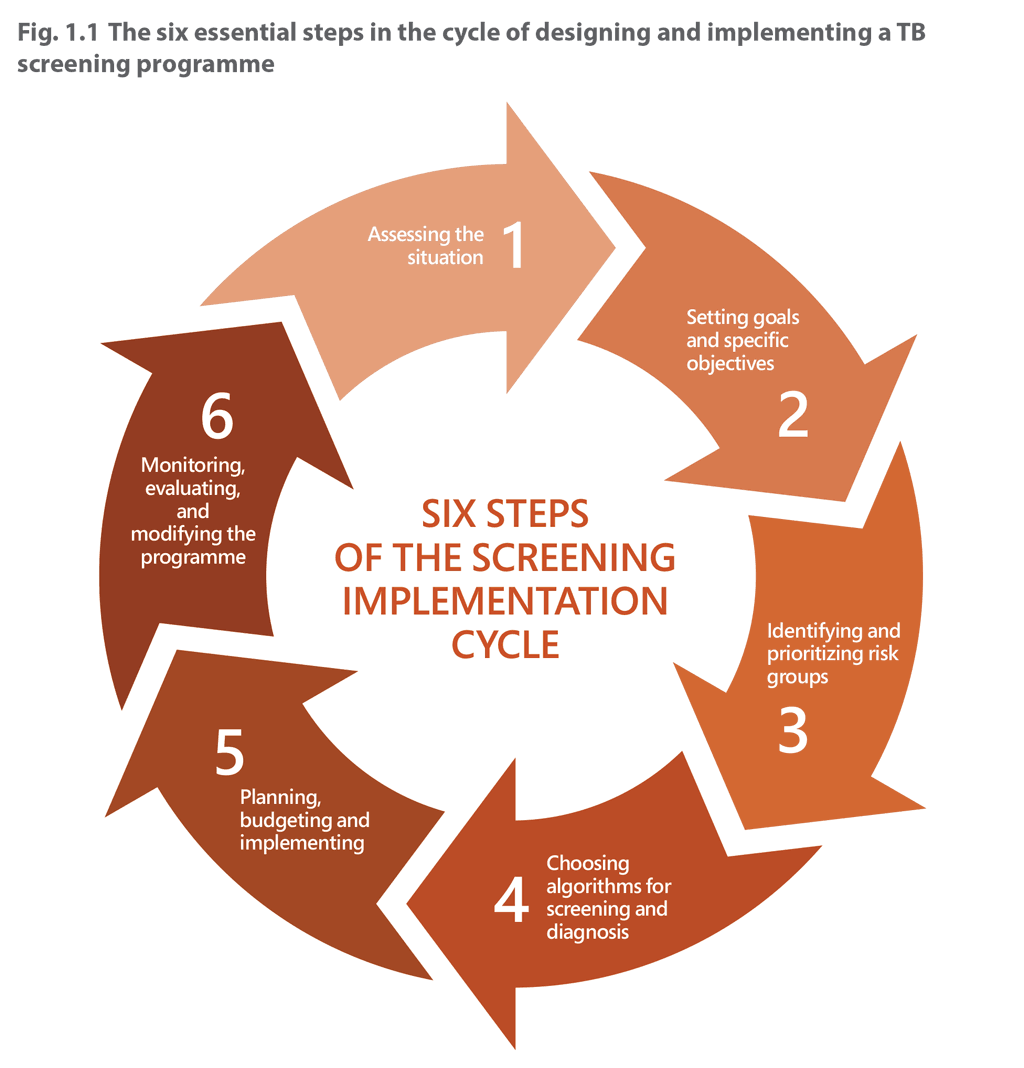
Six essential steps in the cycle of designing and implementing a TB screening programme are discussed in Chapter 2: 1) assessing the situation; 2) setting goals and specific objectives; 3) identifying and prioritizing risk groups; 4) choosing algorithms for screening and diagnosis; 5) planning, budgeting and implementing and 6) monitoring, evaluating and modifying the programme. These six steps are an iterative process, which may lead to revision of the strategy, as necessary. The process should be followed throughout screening and integrated with overall national TB and health systems activities (Fig. 1.1).
Details of different screening tools and their performance in different populations and of algorithms for screening and diagnosis are described in Chapter 3. Most of the approaches proposed in this handbook are for detecting pulmonary TB, the predominant form of the disease worldwide, which is directly transmissible and for which most evidence exists. This does not diminish the importance of extrapulmonary TB as a public health concern in many countries and in certain subpopulations (e.g. children). About 16% of new and relapsed TB patients reported globally in 2019 had exclusively extrapulmonary forms of TB, presenting an additional challenge for detection. Screening for extrapulmonary TB is therefore an important gap that should be filled by research and guidance. The screening tools described here include assessment of symptoms and chest X-ray (CXR), which have traditionally been used for TB screening, and tools that are newly recommended for screening, including computer-aided detection (CAD) technologies for automated interpretation of digital CXR, C-reactive protein (CRP) for screening people living with HIV and use of WHO-recommended rapid molecular diagnostic tests (mWRDs) for screening. Algorithms that combine various screening and diagnostic tools in order to optimize accuracy and ensure a feasible implementation strategy are also discussed. As algorithms perform differently in different populations, an online tool, ScreenTB, has been developed to assist in prioritizing risk groups for screening and choice of algorithm. It is described in Chapter 3.
CAD software packages for automated interpretation of digital CXR images of TB are recommended for screening for the first time by WHO. Chapter 4 provides suggestions on implementation of CAD technologies in new settings, including selection of CAD technologies and protocols for operational research to facilitate implementation. This chapter also provides a description of an online tool, CAD for TB, for the analysis and interpretation of data for CAD calibration. Chapter 5 specifically addresses TB screening in people living with HIV, describing the different subpopulations (outpatients receiving antiretroviral treatment (ART), outpatients newly enrolling in ART care, inpatients with HIV and pregnant women living with HIV), who have specific needs and in whom screening tests perform differently. Because new screening tools are recommended for TB screening in people living with HIV, including CRP and mWRD, specific consideration is given to how these tools and associated algorithms might be integrated into HIV services with additional tests like lateral flow urine lipoarabinomannan assay (LF-LAM) for people with advanced disease.
Chapter 6 addresses operational factors specific to the new recommendations on screening in children, including a discussion of implementation specifically for different subpopulations of children by age group and risk population.
 Feedback
Feedback