Book traversal links for 6.4.3. Implementation considerations
Generally, integration of TB care and treatment into DSD models requires adaptations at multiple levels of the health system, including national, facility and community levels (177). This includes enhancement of leadership and coordination, adaptation of guidelines, capacity-building, adjustments in logistics management, alignment of existing recording and reporting tools, and community engagement. Other factors to consider include the local burden of HIV and TB disease, existing infrastructure and
human resources.
The WHO policy on collaborative TB/HIV activities recommends the delivery of integrated TB and HIV services, preferably at the same time and location, to improve access to good-quality services (167). Advances in HIV care and treatment towards the provision of differentiated services imply that NTPs must work closely with HIV programmes to ensure TB services are integrated into all the DSD models of care.
DSD models for HIV treatment are described within one of the following four categories:
- group models managed by HCWs;
- group models managed by clients;
- individual models based at facilities;
- individual models not based at facilities.
This implies there is a need to enhance capacity for provision of TB services within DSD models, such as training, mentorship and supportive supervision. Client-driven DSD models allow for task-shifting, and it is important for NTPs to clearly map out the tasks that can be provided by lay providers within the DSD model.
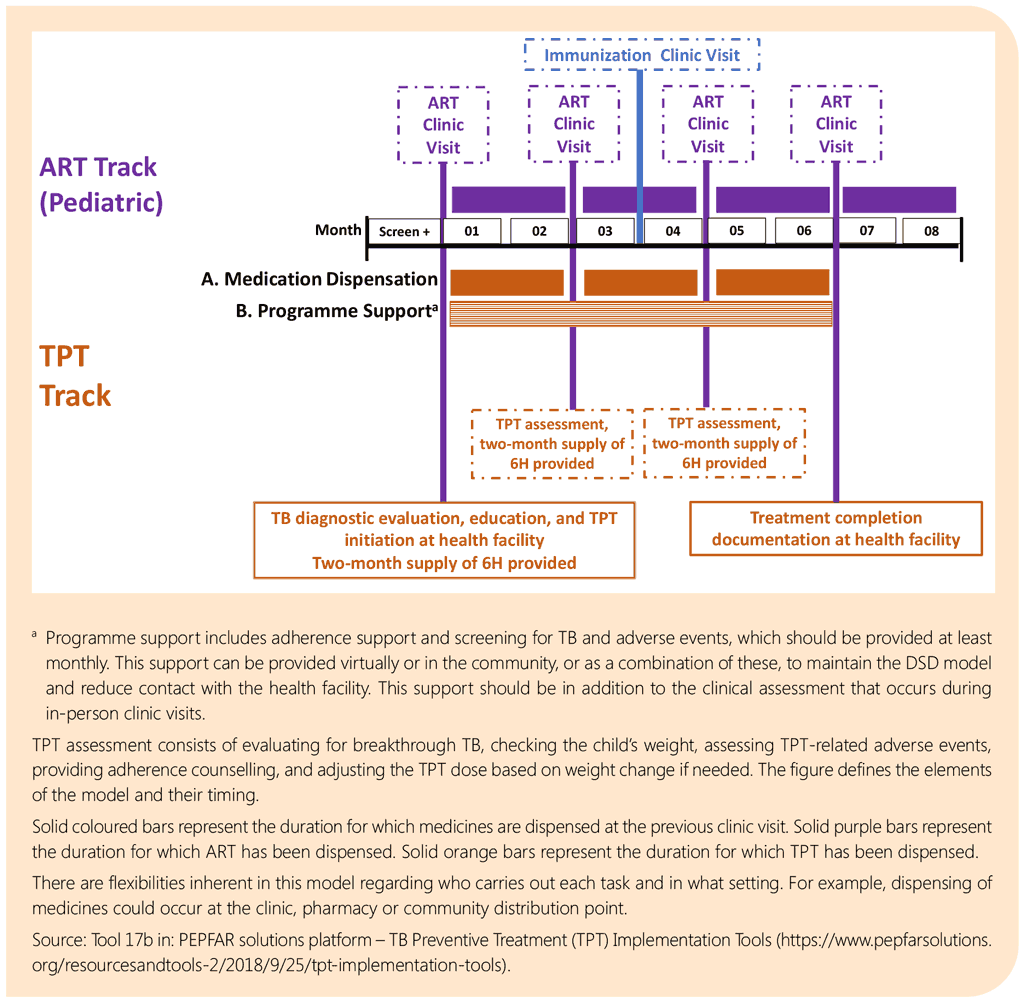
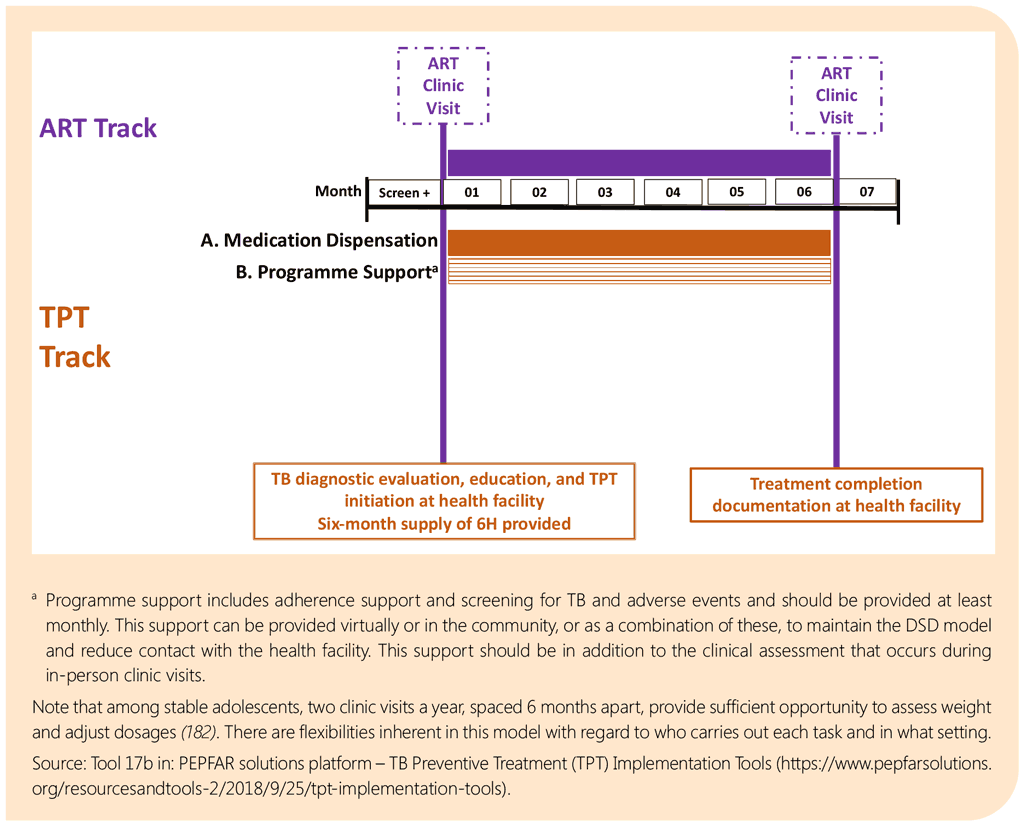
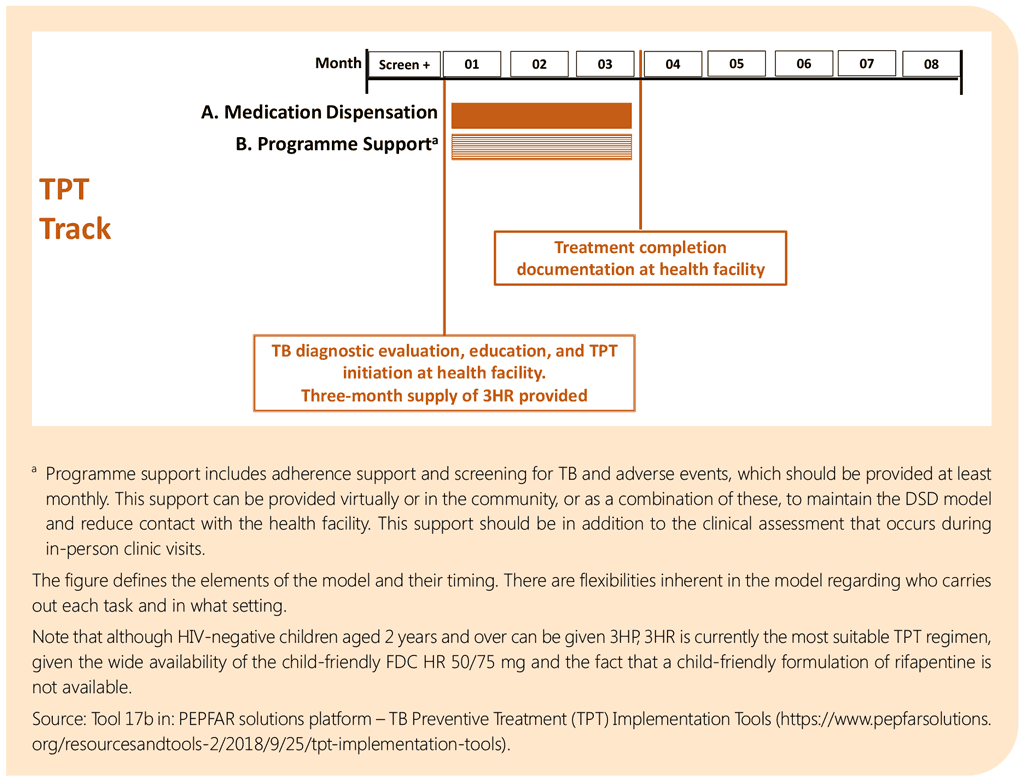
DSD for HIV treatment aims to separate clinical consultations from other visits, such as for ART refills or psychosocial support. Such components need to be taken into consideration as TB services are being provided for within the DSD models. DSD models such as multimonth dispensing of ART would require adjustments in dispensing of TB or TPT medicines, including for children and adolescents, to ensure alignment with medicine refills. Adherence support mechanisms and platforms, including digital adherence technologies, to monitor adverse events of ART can be leveraged to enhance TB treatment completion. Family-centred models for ART that include children and their parents or caregivers can also incorporate TPT and may improve clinical outcomes for the entire family and reduce unnecessary travel and costs.
TB treatment follow-up processes such as weight monitoring to guide dose adjustments are critical and should be catered for. On the other hand, the multimonth dispensing approach may require fewer visits to service delivery points, which may translate into fewer opportunities for TB screening or reduced quality of TB screening. Similarly, failure to align TB and HIV services within the models may lead to treatment interruption resulting from complex follow-up schedules. Data capture and reporting mechanisms for TB care processes and outcomes, especially within the models that are not managed by health workers and those not based at the health facility, are important.



 Feedback
Feedback