Book traversal links for 5.2.2 C-reactive protein (CRP)

C-reactive protein (CRP) is an indicator of systemic inflammation that can be measured with a blood test. A point-of-care test is available that is performed on capillary blood collected from a finger-prick, making it simple, affordable and feasible in primary care. The turnaround time from testing to result with many CRP test kits is 3–5 min, allowing a quick clinical decision to refer a patient for diagnostic evaluation for TB disease or initiation of TPT. An additional potential benefit of CRP is that it can alert clinicians to the presence of other diseases, such as bacterial pneumonia, bronchitis or other infectious or non-infectious conditions (e.g. lymphoma). Health staff and patients may be more confident in the results of a biochemical test than of a more subjective symptom screen.
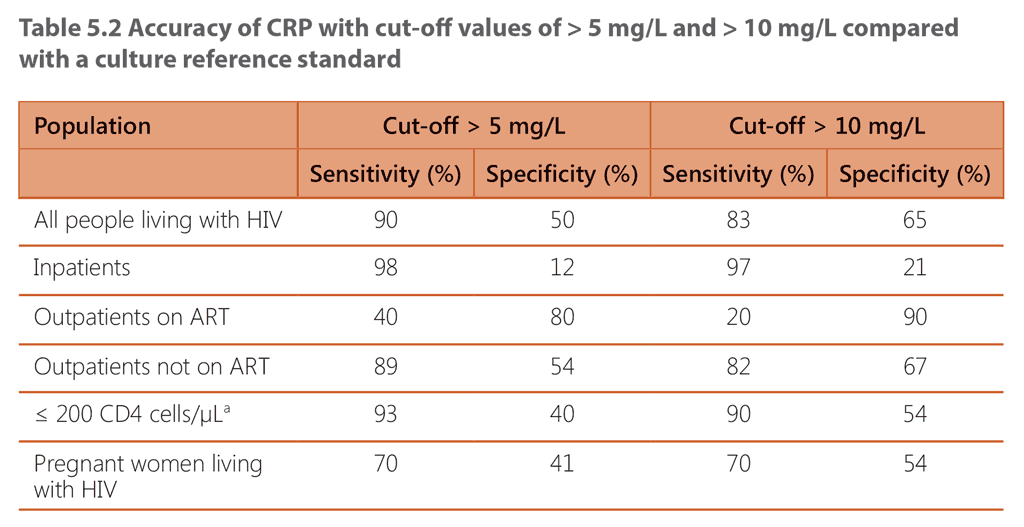
The threshold for considering a result as abnormal may differ by setting. Evidence for the use of a cut-off value of > 5 mg/L or > 10 mg/L was reviewed for the screening guideline; both were found to have the necessary accuracy for detecting TB disease. Currently, the cut-off value of > 5 mg/L is recommended, as it is the lowest threshold indicating abnormality in many clinical settings and because it is the most sensitive. At this cut-off, CRP has a similar sensitivity and higher or similar specificity to symptom screening in all subpopulations of adults and adolescents living with HIV tested (Table 5.2, and see Web Annex B of the screening guidelines). CRP shows clinically significantly greater sensitivity and specificity than W4SS among outpatients living with HIV who are not on ART (CRP, sensitivity 89% and specificity 54%; W4SS, sensitivity 84% and specificity 37%). CRP can also be used in combination with W4SS. While a parallel approach will have resource implications because of the higher sensitivity and lower specificity, data reviewed for the 2021 guideline revision support sequential combination of a positive W4SS followed by CRP with a cut-off of > 5 mg/L, particularly for people not on ART (see 5.4, and Web Annex B of the screening guidelines).
CRP can play an important role in ruling out TB disease before initiation of TPT, which is essential in this population, and requires a test with the highest possible negative predictive value. CRP with a cut-off of > 5 mg/L had a negative predictive value of 99.8% among outpatients not on ART in a setting with a 1% prevalence of TB.
For more detail, see Web Annex B of the screening guidelines.
ᵃ Indicator of advanced HIV disease
 Feedback
Feedback