Book traversal links for 5.4.2. Post-TB meningitis in children and adolescents
TBM is the most debilitating form of TB in children. It has high rates of neurological sequalae despite cure and disproportionately affects children aged under 5 years (4, 134). The pooled risk for neurological sequelae in children with TBM was approximately 50% in a systematic review of treatment outcomes, with more advanced clinical stage of disease at diagnosis (stages 2a/b and 3) associated with worse outcomes at the end of treatment (94). Severe functional and neurocognitive disability is seen in 12–26% of children with TBM and requires long-term care and support (95, 96, 135, 136). The outcomes of children who survive TBM into adulthood are not well documented. Information on long-term neurocognitive, functional and behavioural impairment is lacking. Various instruments have been developed for the standardized assessment of neurodevelopmental, neurocognitive, functional and neurobehavioural outcomes or impairments related to TBM based on age, domains tested and type of test (performance-based, self or caregiver rating).
Annex 7 provides an overview of options for neurocognitive and functional testing at the end of treatment and beyond, including throughout schooling, where resources permit (137). Neuroimaging is usually not indicated as there is a poor correlation between imaging findings at the end of treatment and developmental outcomes (138).
Approximately 80% of children with TBM stage 2 or 3 have hydrocephalus, and 20% of these have a non-communicating type that requires ventriculoperitoneal shunting, for which review every 6 months for possible shunt dysfunction is required. Physiotherapists or occupational therapists should be involved to assess and manage muscle tone and the need for transport (e.g. use of a wheelchair).
Children with severe disabling sequelae should be assessed by a multidisciplinary team for general clinical care requirements post-TBM, including pain management. There should also be end-of treatment assessment for feeding options such as percutaneous gastrostomy with or without gastric fundoplication to relieve gastro-oesophageal reflux.
Approximately 15% of people who survive TBM are completely or partially blind (139). The main causes are chronically raised intracranial pressure (hydrocephalus or tuberculomas), direct involvement of the optic chiasm or optic nerves, and vasculitis related to occipital infarction. Regular evaluation of vision (visual acuity and fields) and promotion of eye health is recommended.
Hypopituitarism due to lesions affecting the hypothalamus, pituitary stalk or the pituitary have been described in 20% of children, often years after recovery from TBM (140). Early recognition of growth restriction, precocious puberty and obesity is beneficial.
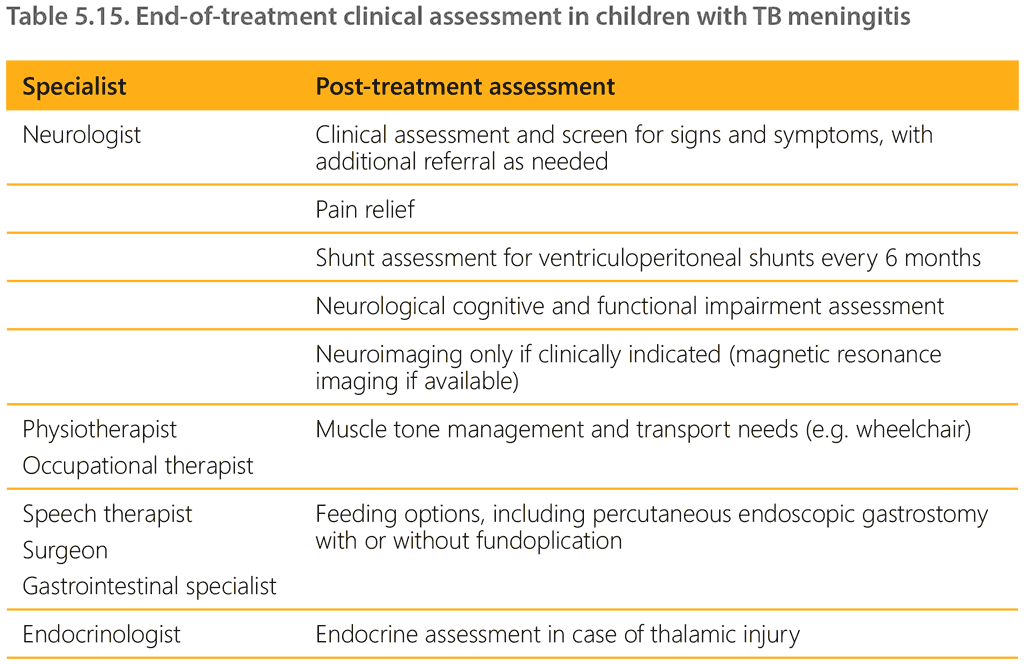
Table 5.15 summarizes end-of-treatment clinical assessment in children with TBM.
 Feedback
Feedback