Book traversal links for 5.3.2.5. Special considerations: TB meningitis
Recommendations on longer MDR/RR-TB treatment regimens for adults also apply to children and adolescents with severe forms of extrapulmonary MDR/RR-TB, as they are not eligible for the short all-oral bedaquiline-containing regimen. In addition to the principles described above, treatment of MDR/RR-TBM should be guided by the ability of the medicines to cross the blood–brain barrier and resulting CSF concentrations, where this is known (Table 5.13).
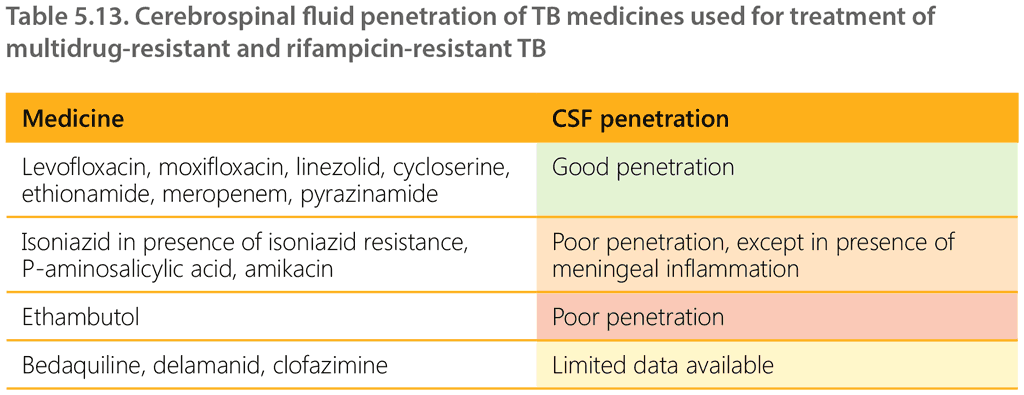
Medicines that should generally be prioritized for treatment of MDR/RR-TB TBM because of their good CSF penetration include the fluoroquinolones (levofloxacin, moxifloxacin), linezolid, cycloserine/terizidone and ethionamide (if there is likely to be susceptibility). Regimens for people with MDR/RR-TB TBM ideally should include at least three medicines with good CSF penetration; additional medicines should then be added following the principles described above to construct a regimen that considers the severity of disease. For example, the addition of bedaquiline should be considered
if there is pulmonary disease in addition to CNS disease.
Although shorter durations of linezolid may be appropriate in many cases of pulmonary MDR/RR-TB, treating MDR/RR-TB TBM with linezolid for longer durations, including possibly throughout the treatment duration, is advisable if tolerated, given its good CSF penetration and the lack of other good treatment options.
Most other forms of extrapulmonary MDR/RR-TB can be treated similarly to pulmonary MDR/RR-TB using the longer regimen. Osteoarticular (including spinal) MDR/RR-TB is usually treated for at least 18 months because of uncertainty regarding bone penetration of TB medicines and since this type of extrapulmonary disease is considered severe.
 Feedback
Feedback