Book traversal links for 1.5. Structure of the operational handbook
The chapters in the handbook are structured around the pathway of TB infection and disease in an individual child or adolescent and the interface with and retention across sequential stages of care (cascade of care), as shown in Figure 1.1 (5).
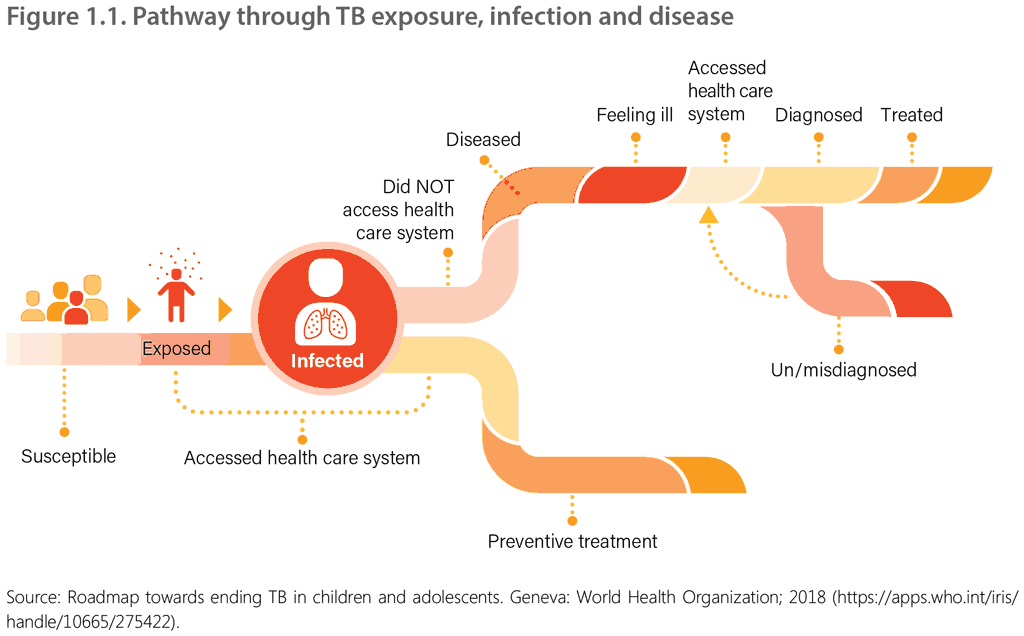
The pathway involves multiple steps, from exposure to a person with an infectious form of TB, leading to subsequent TB infection and, for some people, progression to TB disease. Each of the steps requires evidence-based interventions to reduce TB transmission, prevent TB disease, enable early and accurate diagnosis of TB disease, and optimize treatment outcomes for children and adolescents with drug-susceptible TB or drug-resistant tuberculosis (DR-TB). The steps should take place in the context of child-, adolescent- and family-friendly health care services.
Chapter 2 covers TB screening and contact investigation as the first step in the cascade of care. Chapter 3 on TB prevention in children and adolescents covers bacille Calmette-Guérin (BCG) vaccination, TPT and TB infection prevention and control. Chapter 4 covers the diagnosis of pulmonary tuberculosis (PTB) and extrapulmonary tuberculosis (EPTB) (both drug-susceptible and drug-resistant forms), including the use of diagnostic tests and how to make a decision to start TB treatment based on integrated treatment decision algorithms for use in different settings. The chapters on the cascade of care conclude with Chapter 5 on the treatment of drug-susceptible and drug-resistant PTB and EPTB, with a section on post-TB health. Figure 1.1 is presented at the beginning of each chapter, highlighting the part of the pathway being addressed by the chapter. Chapter 6 covers models of care to improve TB service delivery in line with the special needs of children, adolescents and families.
Chapter 7 is on special situations and provides practical guidance on the management of TB in children and adolescents living with HIV; TB in pregnancy and management of babies born to women with TB disease; palliative care for children and adolescents with TB; care for adolescents with or at risk of TB; TB in children with pneumonia; and TB in children with malnutrition.
The annexes include resources, practical tools and standard operating procedures.
Recommendations for which this operational handbook provides operational guidance use the strength (and quality of evidence) as indicated in the consolidated guidelines on the management of TB in children and adolescents (and relevant source guidelines).
A strong recommendation is one for which there is confidence that the desirable effects clearly outweigh the undesirable effects. In this case, the recommendation is formulated using the word “should”.
A conditional recommendation is one for which the guideline development group concluded that the desirable effects probably outweigh the undesirable effects or are closely balanced, but the group was not confident about these trade-offs in all situations. Conditional recommendations are formulated using the word “may” (see web annex 1 of the consolidated guidelines on the management of TB in children and adolescents).
Although the aim is for harmonization of age definitions for children and adolescents, the age cutoffs for recommendations in this handbook were informed by the evidence available at the time it was reviewed and were based on the source guidelines. Throughout the operational handbook, boxes with recommendations are indicated with a green colour, key points are in light blue and examples, case studies and useful resources in light orange.
 Feedback
Feedback