Book traversal links for 4.1 General considerations: integrated and person-centred TB infection cascade of care
The decision by a ministry of health to initiate or expand TB infection testing requires preparedness of medical services. Many of the people who may be eligible for TPT will need to be able to access this important intervention. This means that referral pathways and health services must be planned or reorganized to ensure that all individuals among target populations are tested promptly and linked to appropriate treatment based on the test results. This is best accomplished by adopting a patient-centred approach that considers the individual’s needs and perspectives. Programmes should streamline services to minimize delays and should coordinate delivery of health care services following the suggested simplified cascade of care (Fig. 4.1). Where possible, different activities in the TB infection cascade of care should be merged to reduce the number of visits needed and to integrate screening for TB disease and TB infection so that these two essential activities are performed together. This chapter reviews how NTPs should organize health services and plan resource allocation to ensure high-quality integrated and person-centred care for all steps of the TB infection cascade of care, to maximize retention in the TB infection cascade.
Fig. 4.1. Simplified four-step person-centred TB infection cascade of care
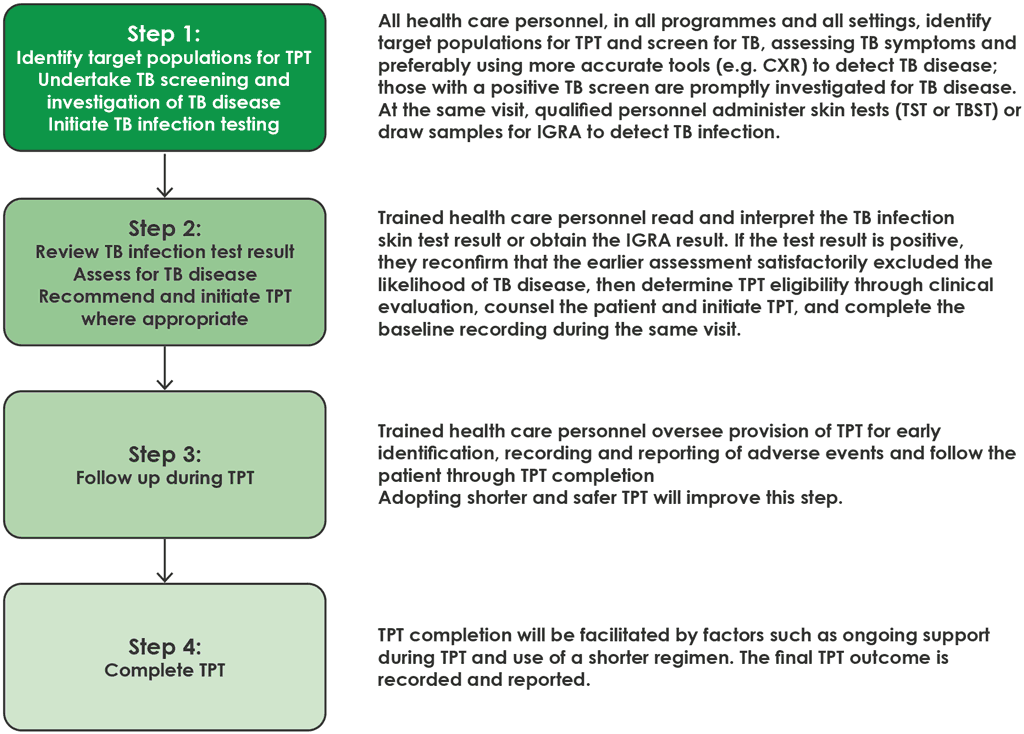
CXR: chest X-ray; IGRA: interferon-gamma release assay; People with HIV: people living with human immunodeficiency virus; TB: tuberculosis; TBST: Mycobacterium tuberculosis antigen-based skin test; TPT: tuberculosis preventive treatment; TST: tuberculin skin test.
The first step of the cascade of care (first health care encounter or visit) is to identify target populations for TPT, and initiate screening for both TB disease and TB infection. This step can be implemented by health care personnel, in health facilities or at home, depending on the organization and resources of the local health system. Standard operating procedures (SOPs) and implementation protocols should be developed for systematic implementation of activities across the cascade of care. Health care personnel in all facilities must be trained to identify and screen priority populations, especially People with HIV and household contacts of TB patients. In addition to these populations, at secondary and tertiary facilities, health care personnel should also actively search for other high-priority groups – for example, transplant candidates, patients with autoimmune disease starting immunosuppressive drugs and patients with cancer starting chemotherapy – according to national policy. Mechanisms should be establishedto ensure that all those at high risk are identified; such mechanisms can include reminders in medical charts, registry books and digital tools, as long as these are regularly checked.
In regard to the first visit (i.e. the initial evaluation of individuals in target population):
- a registered nurse, a nurse aid or a community health agent should ask about TB symptoms (cough, fever, night sweats and weight loss);
- highly accurate screening tools should be used where available; they include CXR (with or without computer-aided detection), WHO-recommended rapid diagnostics or C-reactive protein for People with HIV, as specified in the WHO screening guidelines (28); and
- a TB infection test should be performed – if the TB screen is positive, the person should still have TB infection testing, along with investigations for TB disease initiated on the same day, as specified in the WHO diagnostic guidelines (31).
In regard to the second visit:
- it should occur 48–72 hours after the first visit, and should include reading the TB infection skin test reaction or obtaining the IGRA result; and
- it is required for all those who initially were screened positive for TB disease but in whom TB disease was excluded, and all those who initially screened negative for TB disease:
- if the TB infection test is negative, and the person is well, they can be discharged;
- if the person is initially symptomatic but TB disease has been satisfactorily excluded and the TB infection test is positive, then TPT can be initiated immediately (as per the algorithm in Fig. 2.1 in Chapter 2); and
- if the person is initially screened negative for TB but the TB infection test is positive, then CXR (if not already done in the initial screening) is warranted, with medical evaluation to exclude TB disease – all these activities should be undertaken on the same day, so that TPT can be prescribed during this same visit.
Provision of integrated patient-centred care requires health services to be organized to screen and evaluate further for TB disease and initiate TB infection testing during the first visit. Also, during the second visit, services must be coordinated to deliver test results (TB infection skin test reading or IGRA results), counselling (including for parents or guardians), CXR and medical evaluation. The identification and referral of patients for TB disease screening and TB infection testing, as well as management of those with positive and negative tests, should be part of a well-established written protocol. A qualified and trained provider (usually a nurse or a nurse’s aide) should administer the TB infection skin tests. A qualified phlebotomist (laboratory technician, nurse or nurse’s aide) should collect the blood sample for IGRA.
The NTP or national tuberculosis reference laboratory usually determines which sites will conduct diagnostic testing, based on factors such as epidemiology, geographical considerations, testing workload, availability of qualified staff, efficiency of referral networks and patient access to services. Two tests – QFT-Plus and WANTAI TB-IGRA – can be performed in laboratories equipped with centrifuges and optic densitometers (for ELISA); however, for T-SPOT.TB, the normalization step requires that PBMCs are separated from whole blood and counted, meaning that additional equipment may be required. When considering IGRAs as the test for TB infection, trained phlebotomists are required to draw the blood sample; also required arerapid transport mechanism for samples, to ensure they reach laboratories performing IGRA tests within the timeframe specified in the package insert. There is also an option for centrifugation of blood at smaller laboratories with transport within a specified time to larger laboratory performing IGRA tests. When considering TST or TBST as the test for TB infection and to maximize accessibility, every primary health care clinic should have refrigeration for storage of TB infection skin tests, and personnel trained to administer and read TB infection skin tests.
Programmes should plan patient support and follow-up for TPT. At a minimum, this means follow-up visits during which health care providers evaluate adherence, tolerability and potential adverse events, and reinforce the importance of completing TPT. Missed visits should trigger an active follow-up for the person and treatment support. Services may also include video support or other mHealth technologies such as instant messaging, to enhance TPT completion (such support will require equipment and technical support as well as human resources for follow-up).
The fourth and last step is recording and reporting of TPT outcomes, ideally using an online information system.
 Feedback
Feedback