Book traversal links for 2.7.2 Proposed indicators
Approaches to screening will depend on each group, and intervention-specific indicators should be developed for each approach. In general, however, the data on indicators shown in Fig. 2.5 should be collected for each targeted risk group, such as all close contacts of TB patients or all people living with HIV in care.
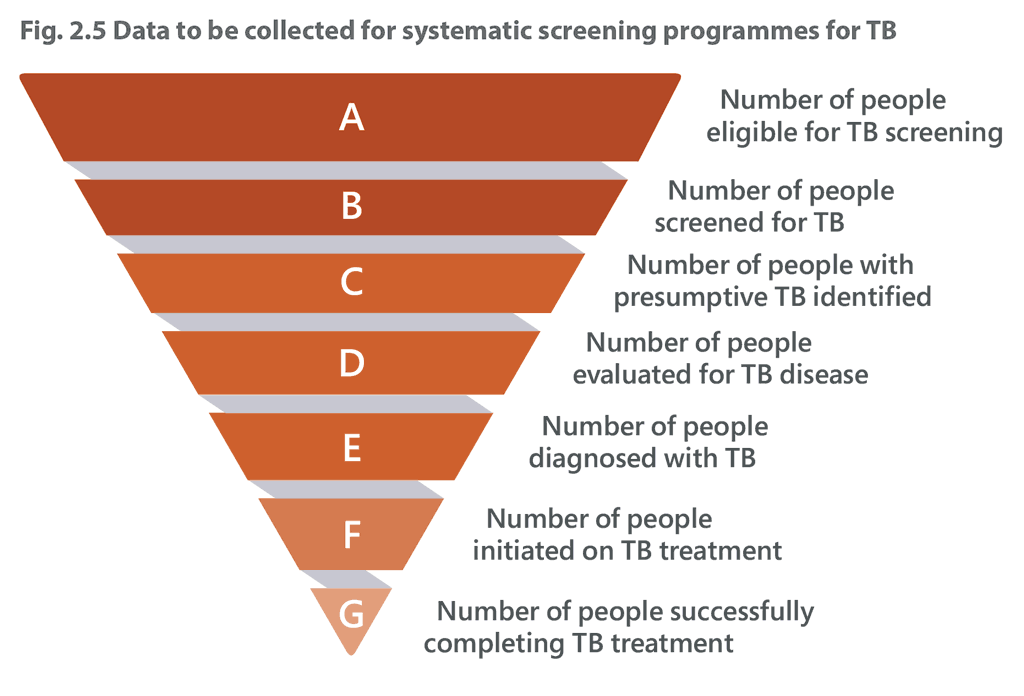
The data collected can be used to calculate the following basic indicators for each risk group:
- acceptability: the proportion of people screened for TB among those eligible (B/A);
- screened positive: the proportion of people presumed to have TB among those screened (C/B);
- testing retention: the proportion of people tested or evaluated for TB with a confirmatory diagnostic test among patients presumed to have TB (D/C);
- NNS and number necessary to treat: the proportion of people diagnosed with TB among those screened (E/B) and tested (E/D);
- linkage to care: the proportion initiating TB treatment among those diagnosed (F/E); and
- treatment success: the proportion of people who successfully complete TB treatment among those who initiated treatment (G/F).
It is critical to monitor the yield of bacteriologically confirmed and unconfirmed TB patients. A high proportion of unconfirmed TB patients referred from screening programmes might indicate overdiagnosis and should lead to closer evaluation of screening and diagnostic routines, considering the limitations of the diagnostic tests and the need for empirical or clinical diagnosis for certain populations, such as people living with HIV and children. In the case of late-stage detection of TB patients, the proportion of people with presumptive TB among those screened (C/B) and the proportion of those diagnosed among those screened (E/B) would be high. This finding would suggest a need for wider active TB case finding in a risk group. Low values for indicators such as the proportion of eligible people screened (B/A), the proportion of those tested who receive diagnostic confirmation (D/C) and the proportion of people diagnosed who start treatment (G/F) may reveal weaknesses in capacity at critical points in the TB care pathway, which should be addressed.
Data should be disaggregated by variables such as age group and sex. This requires collection of some personal data on each individual screened, which should be within the means of most programmes; the necessary software and hardware requirements are relatively modest.
Additional indicators of process (such as the number of people reached and screened per day, the time required for each step of screening and diagnosis and the number of people who require referral) should be collected during the pilot phase of a screening programme to ensure that it operates as designed and to inform logistics and capacity (e.g. number of tests needed). These data are easier to collect precisely than estimates of eligible populations and may indicate problems and can help to plan operational capacity (e.g. screening activities via mobile-vans over time). Once the programme has been established, however, these additional indicators should be discarded and the focus be shifted to streamlining the programme and scaling it up.
The uptake of screening in a risk group (that is, the proportion of those eligible for screening who are actually screened) can be assessed only if the size of the target group has been well defined. It is usually possible to obtain the relevant information for screening conducted in health facilities, closed settings (such as prisons) and through contact investigations; however, it is often difficult to obtain such information in outreach screening programmes, such as when screening is done in the community, although the estimated population of a targeted community provides a rough estimate of the eligible population.
Whenever screening is done, a baseline TB notification rate should be set from historical data, if available (29). These data are usually available to most programmes from notification records. If they are stored in case-based format (or individual patient data), they will permit more extensive disaggregation by the risk groups of interest. Historical data may have to be adjusted for time trends. Screening may generate a substantial yield but with no real change in TB notifications. This could indicate badly located screening points, but may also be the product of better case finding in populations that were previously neglected and a decrease in false-positive cases that previously inflated notification numbers. If this is the case, the proportion of notified TB patients with bacteriologically confirmed disease would be expected to increase over time even if the numbers remain stable.
 Feedback
Feedback