Book traversal links for 7.4 Care for adolescents with or at risk of TB
Adolescents with TB often present with bacteriologically infectious disease typical in adults (e.g. cavities seen on CXR) and therefore pose a high risk for transmission in households and congregate settings such as schools. Adolescents face unique challenges due to peer pressure and fear of stigma, increasing prevalence of comorbidities such as HIV, and risk behaviours such as use of alcohol, tobacco and other substances. People aged 10–19 years need adolescent-friendly services that include relevant psychosocial support and minimal disruption of education (5).
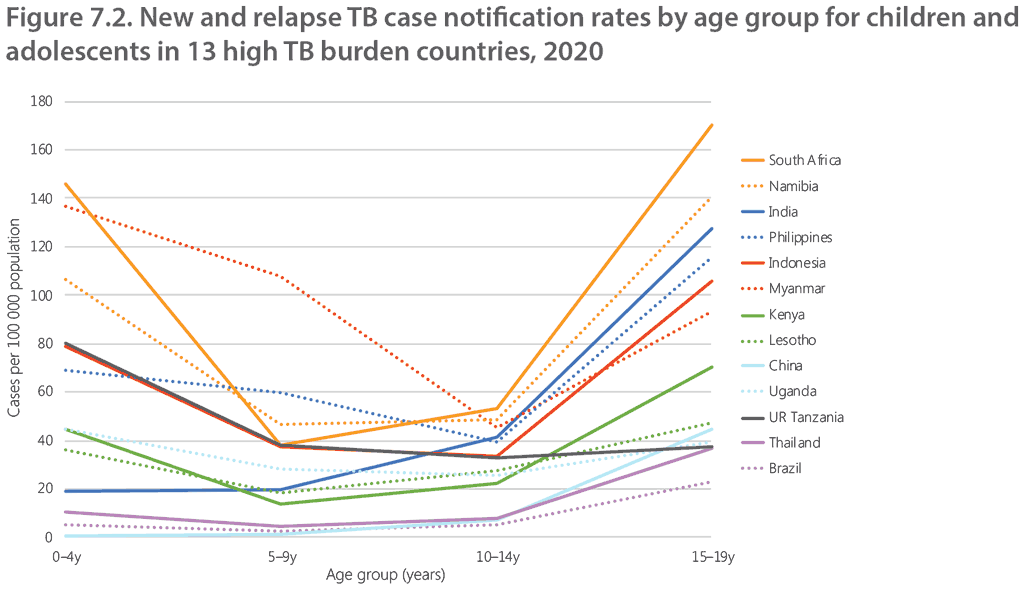
Age-disaggregated data on adolescent TB have been requested by WHO from countries with case-based electronic reporting systems since 2020. Data from 13 high TB burden countries that reported data in 5-year age groups (0–4 years, 5–9 years, 10–14 years, 15–19 years) to WHO for the 2021 Global TB Report show that notification rates in adolescents aged 15–19 years are relatively high compared with younger adolescents (Figure 7.2) (1).
The dynamic physical, psychological, emotional, cognitive and social development that adolescents undergo have implications for their health and well-being. Despite the specific characteristics of this age group, adolescent health data, including on TB, are often grouped together with those of younger children or adults, which means their specific needs, challenges and outcomes are not addressed.
For the evidence review on the background question “How can adolescents with TB or eligible for TPT be optimally engaged in their care?” for the WHO consolidated guidelines on the management of tuberculosis in children and adolescents, the reviewers adapted the five domains of adolescent wellbeing as their theoretical framework (209): good health; connectedness and contribution to society;
safety and a supportive environment; learning, competence, education, skills and employability; and agency and resilience. TB and TB treatment have negative impacts across these five domains.
 Feedback
Feedback