Liens transversaux de livre pour 1. Introduction
1.1 Rationale for TB infection prevention and control
Tuberculosis (TB) continues to be a major public health concern and one of the leading causes of death from a single infectious microorganism at the global level (1). Although recent decades have witnessed increased efforts in the fight to end TB, there are still fundamental systemic gaps, particularly in resource-constrained settings and places with a high TB burden. The World Health Organization (WHO) estimates that about 74 million TB deaths were averted between 2000 and 2021 because of global TB prevention and care efforts. However, about 10.6 million people fell ill with TB in 2021 alone and 1.6 million people died of TB in that year (1).
Although TB can affect everyone, specific population groups have a higher risk of acquiring TB infection or progressing to TB disease once infected (2, 3). These vulnerable populations include people living with HIV, health care workers, children and individuals in congregate settings (e.g. prisons, correction centres, refugee camps and aged care homes). The difficulty and high cost of managing TB disease, especially its drug-resistant forms (4, 5), both to the individual and to the community, underlines the importance of preventing transmission of Mycobacterium tuberculosis within health care facilities, congregate settings, workplaces and the households of TB patients. To achieve the global targets and end the TB epidemic, it is vital to break the chain of M. tuberculosis transmission (6, 7); this requires rapid identification of individuals who have TB disease, prompt treatment and preventive treatment of those at risk, limiting exposure to individuals who may transmit M. tuberculosis and reducing the concentration of infectious particles in the ambient air. In programmatic settings, implementation of these TB infection prevention and control (IPC) interventions (5, 8) is currently lacking, particularly in countries with a high burden of TB and HIV, owing to competing priorities for ministries of health (MoHs). To implement TB IPC guidelines, TB IPC interventions must be prioritized, human and financial resources must be allocated, and there must be systematic engagement with the broader health system and other line ministries within national governments.
One of the targets of the United Nations Sustainable Development Goals (SDGs) for 2015–2030 is to end the global TB epidemic. Therefore, the WHO End TB Strategy, which was approved by the World Health Assembly in 2014, calls for a 90% reduction in TB deaths and an 80% decrease in the TB incidence rate by 2030 compared with 2015 (9). The strategy emphasizes the need to strengthen TB prevention efforts across its three pillars, including TB IPC in health care facilities and settings with a high risk of transmission of M. tuberculosis. In 1999, WHO published recommendations for TB IPC in health care facilities in resource-limited settings (10); these recommendations were expanded in 2009 to provide specific guidance on interventions at health care facilities, in congregate settings and in households (11). A framework for the implementation of TB infection control measures was also developed, to complement the 2009 WHO policy document (12). In 2019, WHO published updated and consolidated guidelines on TB IPC, based on the latest evidence and linked with the core components of general IPC programmes, published in 2016 (13).
1.2 Objective and target audience
The objective of this handbook is to provide practical advice on how to implement the WHO recommendations on TB IPC within the clinical and programmatic management of TB, using a public health approach. This handbook emphasizes the importance of building integrated, well-coordinated, multisectoral actions across all levels of health care and other settings where there is a high risk of M. tuberculosis transmission. It shares best practices and experiences and provides checklists and job aids to support the implementation and monitoring of actions to cut transmissions. There is also an inherent risk of transmission of M. tuberculosis in congregate settings. This document promotes the implementation of a hierarchy of TB IPC interventions across all settings and emphasizes the importance of implementing an integrated package of interventions.
The target audience for this document includes policy-makers at national and subnational level; programme managers for TB, HIV and noncommunicable disease (NCD) programmes; managers and clinicians at inpatient and outpatient health care facilities; managers at various congregate settings; occupational health officials; engineers; medical practitioners; frontline health care workers; and other key stakeholders in the public and private sectors. This document does not cover TB laboratory biosafety or airborne infection control in the context of coronavirus disease 2019 (COVID-19); these topics are covered in other resources (14, 15).
1.3 Adopting the core principles of IPC in TB programmes
Before discussing TB-specific measures in more detail, it is important to consider how universal principles of IPC apply to TB IPC. MoHs should embed TB IPC interventions within the broader framework of IPC, from the national to the facility level. In 2016, WHO issued a set of guidelines identifying eight core components of IPC (16) based on the most recent evidence. The aim was to address the current threats posed by infectious disease and to prevent future threats by strengthening health system resilience and combating antimicrobial resistance (AMR). The 2016 guidelines are also intended to support countries in the development of their own national protocols for IPC. The eight core components in the 2016 guidelines include 11 recommendations and three good practice statements developed in a separate WHO guideline development process (17). These are summarized in Fig. 1.1 and Table 1.1. They provide a broader health systems framework for the implementation of IPC. Although the core components in the 2016 IPC guidelines focus on the prevention of hospital-acquired infections, infections with epidemic potential and AMR, the underlying principles apply to all IPC programmes, including the actions aimed at preventing and reducing TB in health facilities and congregate settings. The core components were considered by the WHO guideline development group (GDG) when formulating their recommendations for the 2019 TB IPC guidelines.
Table 1.1. Core components of a national IPC programme, including recommendations and good practices
Core component 1. IPC programmes
1a. Health care facility level
The panel recommends that an IPC programme with a dedicated, trained team should be in place in each acute health care facility for the purpose of preventing HAIs and combating AMR through IPC good practices.
(Strong recommendation, very low quality of evidence)
1b. National level
Active, standalone, national IPC programmes with clearly defined objectives, functions and activities should be established for the purpose of preventing HAIs and combating AMR through IPC good practices. National IPC programmes should be linked with other relevant national and professional organizations.
(Good practice statement)
Core component 2. National and facility-level IPC guidelines
The panel recommends that evidence-based guidelines should be developed and implemented for the purpose of reducing HAI and AMR. The education and training of relevant health care workers on the guideline recommendations and the monitoring of adherence with guideline recommendations should be undertaken to achieve successful implementation.
(Strong recommendation, very low quality of evidence)
Core component 3. IPC education and training
3a. Health care facility level
The panel recommends that IPC education should be in place for all health care workers by utilizing team- and task-based strategies that are participatory and include bedside and simulation training to reduce the risk of HAI and AMR.
(Strong recommendation, very low quality of evidence)
3b. National level
The national IPC programme should support the education and training of the health workforce as one of its core functions.
(Good practice statement)
Core component 4. Health care-associated infection surveillance
4a. Health care facility level
The panel recommends that facility-based HAI surveillance should be performed to guide IPC interventions and detect outbreaks, including AMR surveillance, with timely feedback of results to health care workers and stakeholders is essential and should be carried out through national networks.
(Strong recommendation, very low quality of evidence)
4b. National level
The panel recommends that national HAI surveillance programmes and networks that include mechanisms for timely data feedback and with the potential to be used for benchmarking purposes should be established to reduce HAI and AMR.
(Strong recommendation, very low quality of evidence)
Core component 5. Multimodal strategies for implementing IPC activities
5a. Health care facility level
The panel recommends that IPC activities using multimodal strategies should be implemented to improve practices and reduce HAIs and AMR.
(Strong recommendation, low quality of evidence)
5b. National level
The panel recommends that national IPC programmes should coordinate and facilitate the implementation of IPC activities through multimodal strategies on a nationwide or subnational level.
(Strong recommendation, low quality of evidence)
Core component 6. Monitoring/audit of IPC practices and feedback and control activities
6a. Health care facility level
The panel recommends that regular monitoring/audit and timely feedback of health care practices, according to IPC standards should be performed to prevent and control HAI and AMR at the health care facility level. Feedback should be provided to all audited persons and relevant staff
(Strong recommendation, low quality of evidence)
6b. National level
The panel recommends that a national IPC monitoring and evaluation programme should be established to assess the extent to which standards are being met and activities are being performed according to the programme’s goals and objectives. Hand hygiene monitoring with feedback should be considered as a key performance indicator at the national level.
(Strong recommendation, moderate quality of evidence)
Core component 7. Workload, staffing and bed occupancy at the facility level
The panel recommends that the following elements should be adhered to in order to reduce the risk of HAI and the spread of AMR: (1) bed occupancy should not exceed the standard capacity of the facility; (2) health care worker staffing levels should be adequately assigned according to patient workload.
(Strong recommendation, very low quality of evidence)
Core component 8. Built environment, materials and equipment for IPC at the facility level
8a. General principles
Patient-care activities should be undertaken in a clean or hygienic environment that facilitates practices related to the prevention and control of HAI, as well as AMR, including all elements around the WASH infrastructure and services and the availability of appropriate IPC materials and equipment.
(Good practice statement)
8b. Materials, equipment, and ergonomics for appropriate hand hygiene
The panel recommends that materials and equipment to perform appropriate hand hygiene should be readily available at the point of care.
(Strong recommendation, very low quality of evidence)
AMR: antimicrobial resistance; HAI: health-care-associated infection; IPC: infection prevention and control; WASH: water, sanitation and hygiene.
Fig. 1.1. Core components of WHO IPC
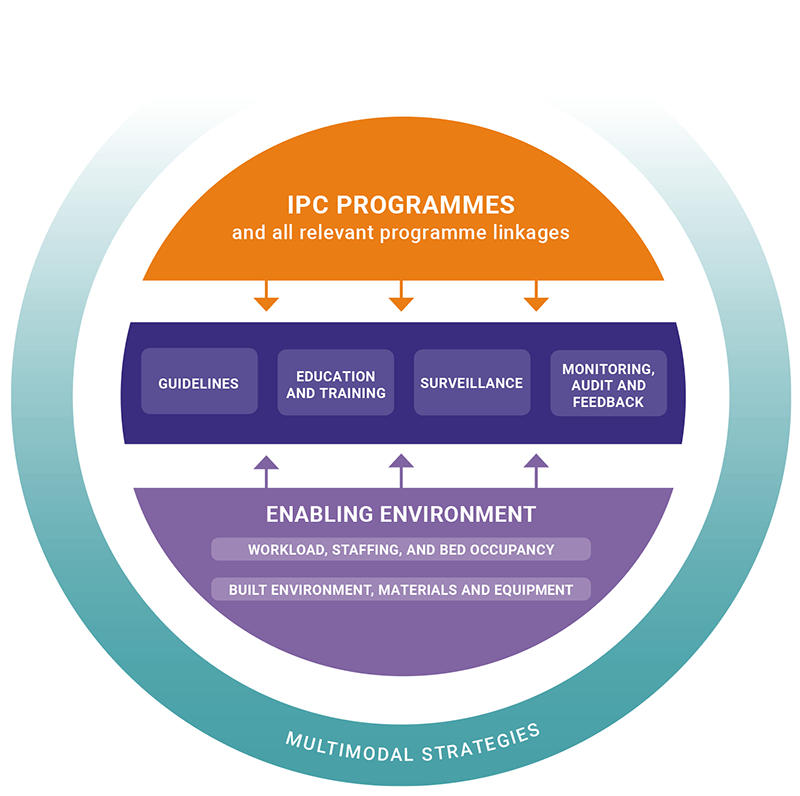
IPC: infection prevention and control; WHO: World Health Organization.
Source: WHO (2019) (17).
The following paragraphs provide suggestions on how countries can integrate TB-specific actions into broader national IPC programmes for each of the core components.
Core component 1, IPC programmes: Health facilities may already have IPC committees that have relevant expertise (e.g. in blood transfusion safety, hepatitis and other bloodborne infections, and infections after general and orthopaedic surgery, delivery and postpartum). The IPC committees often work in isolation and do not prioritize control of airborne infections such as TB. Therefore, the MoH should ensure that IPC committees prioritize TB IPC and systematically incorporate it into their mandate at all levels. A TB focal person should be included on all IPC committees across the health system.
Core component 2, IPC guidelines: The MoH should ensure that TB IPC recommendations are adequately reflected in the national IPC guidelines, implementation protocols and standard operating procedures (SOPs), to facilitate systematic implementation across all levels of health services.
Core component 3, Education and training: Training and on-the-job education of health care workers and facility staff should include training in the TB IPC recommendations. Furthermore, standard education tools (e.g. posters and flow charts targeting staff, patients and visitors to the health facilities or congregate settings) should cover actions for TB IPC. The facility’s focal person for TB IPC should facilitate the training and education of staff and visitors on TB IPC actions.
Core component 4, HAI infection surveillance: Central to the successful implementation of TB IPC are surveillance of the TB burden at the facility, national and subnational levels, and provision of timely feedback to staff. MoHs should also ensure that key data variables related to TB IPC interventions are systematically reviewed at all levels (see also Chapter 6 and Annex 1). TB among health workers is a proxy indicator for the quality of TB IPC actions in a health care facility or congregate setting (18). This calls for the establishment of a programme for periodic screening of health workers or staff for TB, rapid identification of TB disease, notification, and prompt start of TB treatment.
Core component 5, Multimodal strategies for implementing activities: The following multimodal strategies were applied in the studies reviewed by the GDG for the 2016 WHO IPC guidelines (6, 7, 16):
- system change – that is, the availability of the appropriate infrastructure and supplies to implement IPC good practices.
- education and training of health workers and key stakeholders (e.g. facility managers);
- increased accountability via monitoring and timely feedback
- reminders in the workplace; and
- culture change within the establishment (if necessary), with leadership engagement and positive reinforcement strategies to promote practices that ensure patient safety.
Effective integration of TB IPC into each of these strategies, at an appropriate level, should be ensured.
Core component 6, Monitoring/audit and feedback: TB IPC activities should be regularly monitored and aligned with other IPC interventions at the national and local health care facility levels, and feedback should be provided to the staff concerned for quality improvement purposes (see also Chapter 6 and Annex 1). Periodic surveys may also be undertaken to capture data not routinely collected for the monitoring of TB IPC, and to understand the extent of implementation or adherence to national IPC protocols and SOPs.
Core component 7, Workload, staffing and bed occupancy: It is important to limit hospital admission for TB to those with severe disease (e.g. life-threatening conditions, severe adverse events or comorbidities) (6, 7, 16). It is also important to the ensure that sufficient staff are available to serve the number of patients covered by the health facility with high-quality care and effective TB IPC. WHO encourages ambulatory or decentralized and home-based treatment for TB, in preference to inpatient care or isolation (19).
Core component 8, Built environment, materials, and equipment: In the context of TB, this component may imply that respiratory protection equipment should be made available not only to staff but also to visitors. Equipment and tools for disinfection and dilution of ambient air through effective ventilation systems should also be considered.
Key point: TB IPC interventions should be an integral part of the overall national IPC programme.
1.4 WHO recommendations on TB IPC
The 2019 WHO TB IPC guidelines provide four recommendations on administrative controls (Recommendations 1–4), two on environmental controls (Recommendations 5–6) and one on respiratory protection (Recommendation 7) (13). The administrative controls are management measures aimed at reducing the risk of exposure to M. tuberculosis for individuals attending health facilities or a congregate setting. The environmental controls are intended to prevent the spread of infectious droplets and reduce their concentration in the ambient air. Respiratory protection comprises the use of personal protective equipment (PPE) to limit the risk of acquiring M. tuberculosis infection. In addition, as discussed in Section 1.3, the 2019 guidelines include good practice statements that reflect general principles of IPC that apply to TB. The latest recommendations on TB IPC are summarized in Table 1.2. These controls are discussed in detail in Chapters 2–4.
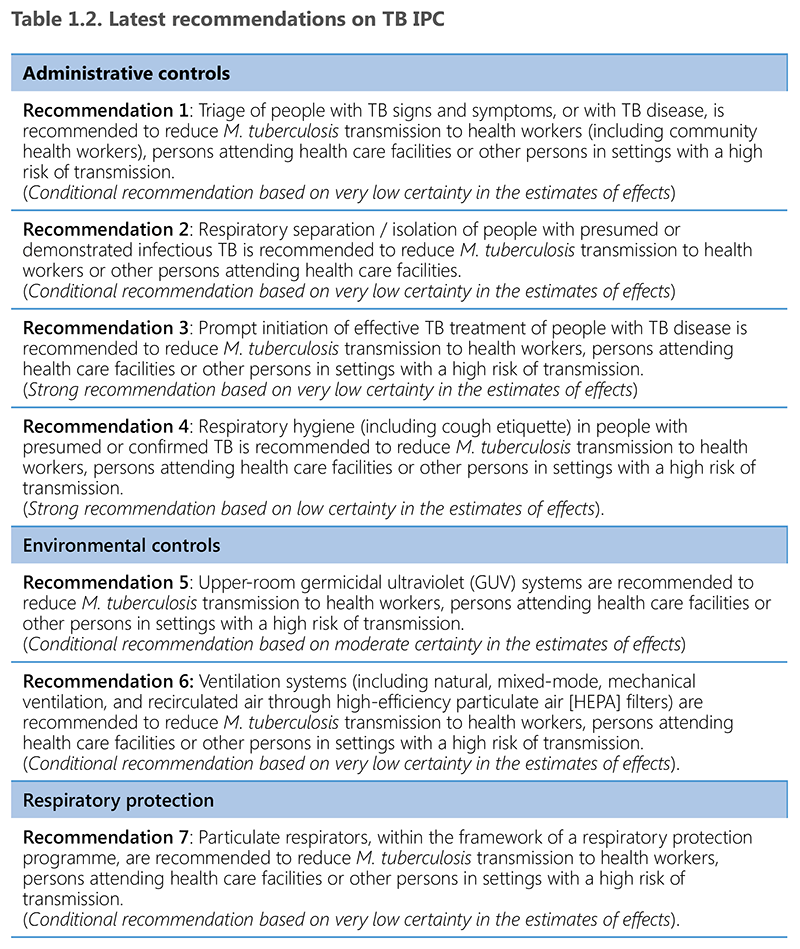
IPC: infection prevention and control; M. tuberculosis; TB: tuberculosis
Source: WHO (2019) (17).
To achieve the optimum impact on TB transmission, the recommended interventions given above should be implemented as a package, not selectively. In settings where there is a high risk of M. tuberculosis transmission, it is important to develop and implement integrated, well-coordinated and multisectoral actions for TB IPC across the health and non-health sectors. These actions should include administrative, environmental, and respiratory control measures, as summarized in Fig. 1.2.
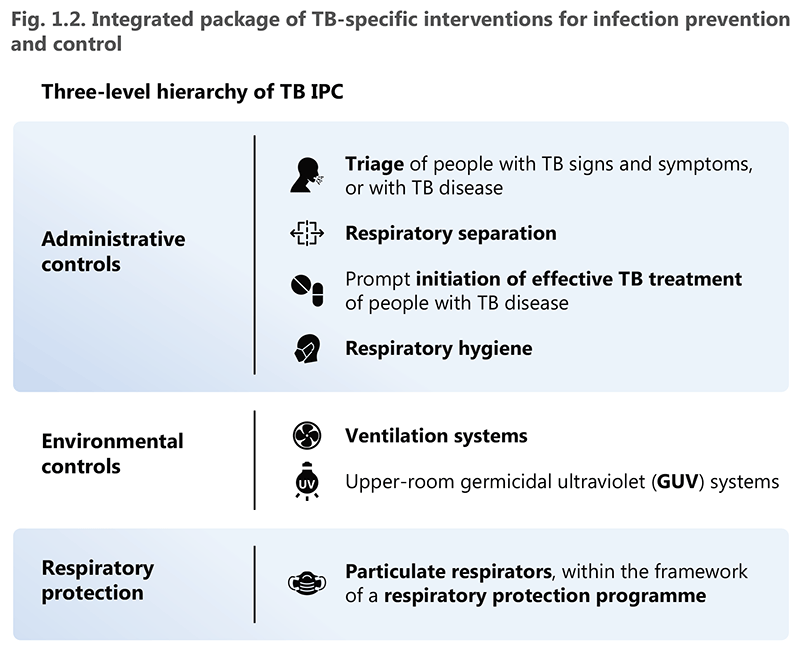
IPC: infection prevention and control; TB: tuberculosis.
Key point: Effective implementation of WHO recommendations on TB IPC relies on interventions within the three-level hierarchy of IPC being implemented as an integrated package (not prioritized individually or implemented separately).
 Retour
Retour